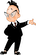Произношение
Общее название: ацетаминофен и трамадол (SEET MIN MIN и TRAM a dol)
Именамарок:Ultracet
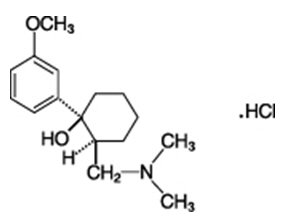
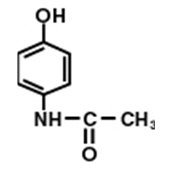
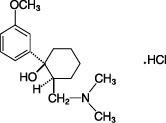
Ultracet содержит комбинацию трамадола и ацетаминофена . Трамадол — наркотик, подобный обезболивающим. Ацетаминофен является менее сильным болеутоляющим средством, которое увеличивает эффекты трамадола.
Ultracet используется для лечения умеренной и сильной боли.
Ultracet также может использоваться для целей, не указанных в данном руководстве.
ЗЛОУПОТРЕБЛЕНИЕ УЛЬТРАКТЕТА МОЖЕТ ПРИВЕСТИ К ПРИКЛЮЧЕНИЮ, ПЕРЕДОЗИРОВКЕ ИЛИ СМЕРТИ, особенно у ребенка или другого лица, использующего лекарство без рецепта.
Не принимайте больше рекомендуемой дозы.
Слайд-шоу Посмотреть страшные (но мертвые серьезные) побочные эффекты лекарств
Вы не должны использовать это лекарство, если у вас серьезные проблемы с дыханием, блокировка в желудке или кишечнике или если вы недавно использовали ингибитор МАО.
Ultracet не одобрен для использования кем-либо моложе 18 лет.
Принятие Ultracet во время беременности может привести к появлению у новорожденных опасных симптомов отмены.
Смертельные побочные эффекты могут возникать, если вы используете Ultracet со спиртом или с другими препаратами, которые вызывают сонливость или замедляют дыхание.
Вы не должны использовать Ultracet, если у вас аллергия на ацетаминофен (Tylenol) или трамадол (Ultram), или если у вас есть:
-
Тяжелая астма или проблемы с дыханием;
-
Закупорка желудка или кишечника; или
-
Если вы использовали ингибиторы МАО (такие как изокарбоксазид, линезолид, фенэлзин, разагилин, селегилин, транилципромин) за последние 14 дней.
Ultracet не одобрен для использования кем-либо моложе 18 лет.
Судороги произошли у некоторых людей, принимающих это лекарство. Ваш риск захвата может быть выше, если вы когда-либо имели:
-
Алкоголизм или наркомания;
-
Эпилепсия или другое нарушение судорог;
-
Метаболическое расстройство;
-
Травма головы или опухоль головного мозга; или
-
Если вы недавно использовали седативные средства, транквилизаторы или наркотические препараты.
Чтобы убедиться, что Ultracet безопасен для вас, сообщите своему врачу, если вы когда-либо имели:
-
Заболевания печени, или если вы пьете алкоголь;
-
Заболевания почек, проблемы с мочеиспусканием;
-
Проблемы с вашей поджелудочной железой, желчным пузырем или щитовидной железой;
-
Депрессия, психическое заболевание или попытка самоубийства; или
-
Если вы используете седативный препарат, такой как валиум (диазепам, альпразолам, лоразепам, ативан, клонопин, ресторил, транксин, стих, ксанак и др.).
Если вы используете Ultracet во время беременности, ваш ребенок может стать зависимым от трамадола. Это может вызвать опасные для жизни симптомы отмены у ребенка после его рождения. Младенцы, рожденные в зависимости от привыкания, могут нуждаться в лечении в течение нескольких недель. Расскажите своему врачу, если вы беременны.
Не кормить грудью. Это лекарство может перейти в грудное молоко и вызвать сонливость, проблемы с дыханием или смерть у кормящих детей.
Возьмите Ultracet точно так, как предписано вашим доктором. Следуйте всем указаниям на этикетке рецепта. Никогда не принимайте это лекарство в больших количествах или дольше, чем предписано. Передозировка может повредить вашу печень или вызвать смерть. Скажите вашему доктору, если лекарство, похоже, перестает работать и облегчает вашу боль.
Максимальная доза Ultracet — 2 таблетки на дозу или 8 таблеток в день. Не принимайте это лекарство более 5 дней подряд.
Ultracet может быть привычной формой, даже при регулярных дозах. Никогда не делитесь им с другим человеком. НЕПРАВИЛЬНОЕ ИСПОЛЬЗОВАНИЕ НАРКОТИЧЕСКОЙ ЛЕКАРСТВЕННОЙ ЛЕКАРСТВЕННОЙ СРЕДЫ МОЖЕТ ПРИВЕСТИ К ПРИКЛЮЧЕНИЮ, ПЕРЕДОЗИРОВКЕ ИЛИ СМЕРТИ, особенно у ребенка или другого лица, использующего лекарство без рецепта. Продажа или раздача этого лекарства противоречит закону.
Вы можете взять Ultracet с едой или без нее, но каждый раз принимайте ее одинаково.
Вы не должны прекращать использование Ultracet внезапно после длительного использования. Следуйте инструкциям своего врача о сужении дозы.
Хранить при комнатной температуре вдали от влаги и тепла.
Следите за своим лекарством. Ultracet является наркотиком злоупотребления, и вы должны знать, кто использует ваше лекарство неправильно или без рецепта.
Обычная доза для взрослых Ultracet для боли:
Обычная доза: 2 таблетки каждые 4-6 часов при необходимости для боли
Максимальная доза: 8 таблеток в день
Максимальная продолжительность: 5 дней
Комментарии:
-Какая таблетка содержит трамадол 37,5 мг и ацетаминофен 325 мг. Максимальная суточная доза составляет Трамадол: 300 мг в день и ацетаминофен 2600 мг в день.
-Использование более 1 продукта в момент времени, содержащий ацетаминофен, не рекомендуется.
Использование: для краткосрочного лечения острой боли; Использование должно быть ограничено до 5 дней или менее.
Обычная гериатрическая доза для боли:
Выбор дозы должен быть осторожным из-за возможности большей чувствительности к нежелательным явлениям.
См. Также: Информация дозирования (более подробно)
Читайте так же про препарат MS Contin.
Поскольку Ultracet используется для боли, вы вряд ли пропустите дозы. Пропустите любую пропущенную дозу, если это почти время для вашей следующей запланированной дозы. Не принимайте дополнительное лекарство, чтобы восполнить пропущенную дозу.
Обратитесь за неотложной медицинской помощью или позвоните в справочную строку Poison по телефону 1-800-222-1222. Передозировка этого лекарства может быть фатальной, особенно у ребенка или другого человека, использующего лекарство без рецепта.
Симптомы передозировки могут включать в себя неглубокое дыхание, медленное сердцебиение, сильную слабость, холодную или липкую кожу, ощущение легкомысленности, обморок, захват или кома.
Читайте так же про препарат Аугментин.
Не употребляйте алкоголь. Могут возникнуть опасные побочные эффекты или смерть.
Избегайте вождения или управления машиной, пока вы не узнаете, как это лекарство повлияет на вас. Головокружение или тяжелая сонливость могут стать причиной падений или других аварий.
Попросите врача или фармацевта перед использованием любого другого лекарства, которое может содержать ацетаминофен (иногда сокращенно APAP). Взятие некоторых препаратов вместе может привести к фатальной передозировке.
Получите неотложную медицинскую помощь, если у вас есть признаки аллергической реакции на Ultracet: ульи; затрудненное дыхание; Отек лица, губ, языка или горла.
Как и другие наркотические лекарства, трамадол может замедлить ваше дыхание. Смерть может произойти, если дыхание становится слишком слабым.
В редких случаях ацетаминофен может вызвать сильную реакцию кожи, которая может быть фатальной. Это могло произойти, даже если вы принимали ацетаминофен в прошлом и не реагировали. Прекратите принимать это лекарство и сразу же позвоните своему врачу, если у вас есть покраснение кожи или сыпь, которая распространяется и вызывает вздутие и шелушение.
Человек, заботящийся о вас, должен обратиться за неотложной медицинской помощью, если у вас медленное дыхание с длинными паузами, губами синего цвета, или если вам трудно проснуться.
Прекратите использование Ultracet и сразу же обратитесь к врачу, если у вас есть:
-
Шумное дыхание, вздох, неглубокое дыхание;
-
Медленный пульс или слабый пульс;
-
Легкомысленное чувство, как вы могли бы исчезнуть;
-
Захват (судороги);
-
грудная боль;
-
Сексуальные проблемы, потеря интереса к сексу;
-
Низкий уровень кортизола — тошнота, рвота, потеря аппетита, головокружение, ухудшение усталости или слабости;
-
Проблемы с печенью — боль в верхнем желудке, потеря аппетита, темная моча, желтуха (пожелтение кожи или глаз); или
-
Высокий уровень серотонина в организме — возбуждение, галлюцинации, лихорадка, быстрый сердечный ритм, сверхактивные рефлексы, тошнота, рвота, диарея, потеря координации, обморок.
Серьезные побочные эффекты могут быть более вероятными у пожилых людей и людей с избыточным весом, недоедания или ослабления.
Долгосрочное применение опиоидных препаратов может повлиять на рождаемость (способность иметь детей) у мужчин или женщин. Неизвестно, являются ли опиоидные эффекты на фертильность постоянными.
Общие побочные эффекты Ultracet могут включать:
-
Головокружение, сонливость, чувство усталости;
-
Боль в желудке, тошнота, потеря аппетита;
-
Диарея, запоры; или
-
потливость.
Это не полный список побочных эффектов, и другие могут возникнуть. Спросите у своего доктора о побочных эффектах. Вы можете сообщить о побочных эффектах FDA на уровне 1-800-FDA-1088.
См. Также: Побочные эффекты (более подробно)
Наркотическое (опиоидное) лекарственное средство может взаимодействовать со многими другими препаратами и вызывать опасные побочные эффекты или смерть. Убедитесь, что ваш врач знает, используете ли вы также:
-
Другие наркотические препараты — лекарство от опиоидной боли или лекарство от кашля по рецепту;
-
Лекарства, которые заставляют вас спать или замедлять дыхание — снотворное, расслабляющий мышцы, успокаивающий, успокаивающий или антипсихотическая медицина; или
-
Лекарства, которые влияют на уровень серотонина в вашем организме — медицина для депрессии, болезнь Паркинсона, головные боли мигрени, серьезные инфекции или профилактика тошноты и рвоты.
Этот список не является полным. Другие препараты могут взаимодействовать с ацетаминофеном и трамадолом, включая рецептурные и внебиржевые лекарства, витамины и растительные продукты. Не все возможные взаимодействия перечислены в данном руководстве по лекарствам.
- Ваш фармацевт может предоставить дополнительную информацию о Ultracet.
1. Indications and Usage for Ultracet
ULTRACET tablets are indicated for the management of acute pain severe enough to require an opioid analgesic and for which alternative treatments are inadequate.
Limitations of Use
ULTRACET tablets are indicated for short-term use of five days or less.
Because of the risks of addiction, abuse, and misuse with opioids, even at recommended doses
[see
Warnings and Precautions (5.1)]
, reserve ULTRACET for use in patients for whom alternative treatment options [e.g., non-opioid analgesics]:
- Have not been tolerated, or are not expected to be tolerated,
- Have not provided adequate analgesia, or are not expected to provide adequate analgesia.
2. Ultracet Dosage and Administration
2.1 Important Dosage and Administration Instructions
- ULTRACET is not approved for use for more than 5 days.
- Do not exceed the recommended dose of ULTRACET. Do not co-administer ULTRACET with other tramadol or acetaminophen containing products
[see
Warnings and Precautions (5.19)]
.
- Use the lowest effective dosage for the shortest duration consistent with individual patient treatment goals
[see
Warnings and Precautions (5.1)]
.
- Initiate the dosing regimen for each patient individually, taking into account the patient’s severity of pain, patient response, prior analgesic treatment experience, and risk factors for addiction, abuse, and misuse
[see
Warnings and Precautions (5.1)]
.
- Monitor patients closely for respiratory depression, especially within the first 24–72 hours of initiating therapy and following dosage increases with ULTRACET and adjust the dosage accordingly
[see
Warnings and Precautions (5.3)]
.
2.2 Patient Access to Naloxone for the Emergency Treatment of Opioid Overdose
Discuss the availability of naloxone for the emergency treatment of opioid overdose with the patient and caregiver and assess the potential need for access to naloxone, both when initiating and renewing treatment with ULTRACET
[see
Warnings and Precautions (5.3),
Patient Counseling Information (17)]
.
Inform patients and caregivers about the various ways to obtain naloxone as permitted by individual state naloxone dispensing and prescribing requirements or guidelines (e.g., by prescription, directly from a pharmacist, or as part of a community-based program).
Consider prescribing naloxone, based on the patient’s risk factors for overdose, such as concomitant use of CNS depressants, a history of opioid use disorder, or prior opioid overdose. However, the presence of risk factors for overdose should not prevent the proper management of pain in any given patient
[see
Warnings and Precautions (5.1,
5.3,
5.8)]
.
Consider prescribing naloxone if the patient has household members (including children) or other close contacts at risk for accidental exposure or overdose.
2.3 Initial Dosage
The initial dose of ULTRACET is 2 tablets every 4 to 6 hours as needed for pain relief up to a maximum of 8 tablets per day.
2.4 Dosage Modification in Patients with Renal Impairment
In patients with creatinine clearances of less than 30 mL/min, do not exceed 2 tablets every 12 hours.
2.5 Safe Reduction or Discontinuation of ULTRACET
Do not abruptly discontinue ULTRACET in patients who may be physically dependent on opioids. Rapid discontinuation of opioid analgesics in patients who are physically dependent on opioids has resulted in serious withdrawal symptoms, uncontrolled pain, and suicide. Rapid discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse. Patients may also attempt to treat their pain or withdrawal symptoms with illicit opioids, such as heroin, and other substances.
When a decision has been made to decrease the dose or discontinue therapy in an opioid-dependent patient taking ULTRACET, there are a variety of factors that should be considered, including the dose of ULTRACET the patient has been taking, the duration of treatment, the type of pain being treated, and the physical and psychological attributes of the patient. It is important to ensure ongoing care of the patient and to agree on an appropriate tapering schedule and follow-up plan so that patient and provider goals and expectations are clear and realistic. When opioid analgesics are being discontinued due to a suspected substance use disorder, evaluate and treat the patient, or refer for evaluation and treatment of the substance use disorder. Treatment should include evidence-based approaches, such as medication assisted treatment of opioid use disorder. Complex patients with comorbid pain and substance use disorders may benefit from referral to a specialist.
There are no standard opioid tapering schedules that are suitable for all patients. Good clinical practice dictates a patient-specific plan to taper the dose of the opioid gradually. For patients on opioids who are physically opioid-dependent, initiate the taper by a small enough increment (e.g., no greater than 10% to 25% of the total daily dose) to avoid withdrawal symptoms, and use a gradual downward taper. Patients who have been taking opioids for briefer periods of time may tolerate a more rapid taper.
It may be necessary to provide the patient with lower dosage strengths to accomplish a successful taper. Reassess the patient frequently to manage pain and withdrawal symptoms, should they emerge. Common withdrawal symptoms include restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other signs and symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate. If withdrawal symptoms arise, it may be necessary to pause the taper for a period of time or raise the dose of the opioid analgesic to the previous dose, and then proceed with a slower taper. In addition, monitor patients for any changes in mood, emergence of suicidal thoughts, or use of other substances.
When managing patients taking opioid analgesics, particularly those who have been treated for a long duration and/or with high doses for chronic pain, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper. A multimodal approach to pain management may optimize the treatment of chronic pain, as well as assist with the successful tapering of the opioid analgesic
[see
Warnings and Precautions (5.20),
Drug Abuse and Dependence (9.3)]
.
3. Dosage Forms and Strengths
ULTRACET tablets each contain 37.5 mg of tramadol hydrochloride and 325 mg of acetaminophen. The tablets are light yellow, coated, capsule-shaped, and debossed with «O-M» on one side and «650» on the other.
4. Contraindications
ULTRACET is contraindicated for:
- all children younger than 12 years of age
[see
Warnings and Precautions (5.4)]
- post-operative management in children younger than 18 years of age following tonsillectomy and/or adenoidectomy
[see
Warnings and Precautions (5.4)]
.
ULTRACET is also contraindicated in patients with:
- Significant respiratory depression
[see
Warnings and Precautions (5.3)]
.
- Acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment
[see
Warnings and Precautions (5.13)]
.
- Patients with known or suspected gastrointestinal obstruction, including paralytic ileus
[see
Warnings and Precautions (5.17)]
.
- Previous hypersensitivity to tramadol, acetaminophen, any other component of this product, or opioids
[see
Warnings and Precautions (5.18)]
.
- Concurrent use of monoamine oxidase inhibitors (MAOIs) or use within the last 14 days
[see
Drug Interactions (7)]
.
5. Warnings and Precautions
5.1 Addiction, Abuse and Misuse
ULTRACET contains tramadol, a Schedule IV controlled substance. As an opioid, ULTRACET exposes users to the risks of addiction, abuse, and misuse
[see
Drug Abuse and Dependence (9)]
.
Although the risk of addiction in any individual is unknown, it can occur in patients appropriately prescribed ULTRACET. Addiction can occur at recommended dosages and if the drug is misused or abused.
Assess each patient’s risk for opioid addiction, abuse, or misuse prior to prescribing ULTRACET, and monitor all patients receiving ULTRACET for the development of these behaviors and conditions. Risks are increased in patients with a personal or family history of substance abuse (including drug or alcohol abuse or addiction) or mental illness (e.g., major depression). The potential for these risks should not, however, prevent the proper management of pain in any given patient. Patients at increased risk may be prescribed opioids such as ULTRACET, but use in such patients necessitates intensive counseling about the risks and proper use of ULTRACET along with intensive monitoring for signs of addiction, abuse, and misuse. Consider prescribing naloxone for the emergency treatment of opioid overdose
[see
Dosage and Administration (2.2),
Warnings and Precautions (5.3)]
.
Opioids are sought by drug abusers and people with addiction disorders and are subject to criminal diversion. Consider these risks when prescribing or dispensing ULTRACET. Strategies to reduce these risks include prescribing the drug in the smallest appropriate quantity and advising the patient on the proper disposal of unused drug
[see
Patient Counseling Information (17)]
. Contact local state professional licensing board or state controlled substances authority for information on how to prevent and detect abuse or diversion of this product.
5.2 Opioid Analgesic Risk Evaluation and Mitigation Strategy (REMS)
To ensure that the benefits of opioid analgesics outweigh the risks of addiction, abuse, and misuse, the Food and Drug Administration (FDA) has required a Risk Evaluation and Mitigation Strategy (REMS) for these products. Under the requirements of the REMS, drug companies with approved opioid analgesic products must make REMS-compliant education programs available to healthcare providers. Healthcare providers are strongly encouraged to do all of the following:
- Complete a REMS-compliant education program offered by an accredited provider of continuing education (CE) or another education program that includes all the elements of the FDA Education Blueprint for Health Care Providers Involved in the Management or Support of Patients with Pain.
- Discuss the safe use, serious risks, and proper storage and disposal of opioid analgesics with patients and/or their caregivers every time these medicines are prescribed. The Patient Counseling Guide (PCG) can be obtained at this link: www.fda.gov/OpioidAnalgesicREMSPCG.
- Emphasize to patients and their caregivers the importance of reading the Medication Guide that they will receive from their pharmacist every time an opioid analgesic is dispensed to them.
- Consider using other tools to improve patient, household, and community safety, such as patient-prescriber agreements that reinforce patient-prescriber responsibilities.
To obtain further information on the opioid analgesic REMS and for a list of accredited
REMS CME/CE, call 1-800-503-0784, or log on to www.opioidanalgesicrems.com.
The FDA Blueprint can be found at www.fda.gov/OpioidAnalgesicREMSBlueprint.
5.3 Life-Threatening Respiratory Depression
Serious, life-threatening, or fatal respiratory depression has been reported with the use of opioids, even when used as recommended. Respiratory depression, if not immediately recognized and treated, may lead to respiratory arrest and death. Management of respiratory depression may include close observation, supportive measures, and use of opioid antagonists, depending on the patient’s clinical status
[see
Overdosage (10)]
. Carbon dioxide (CO
2) retention from opioid-induced respiratory depression can exacerbate the sedating effects of opioids.
While serious, life-threatening, or fatal respiratory depression can occur at any time during the use of ULTRACET, the risk is greatest during the initiation of therapy or following a dosage increase. Monitor patients closely for respiratory depression, especially within the first 24–72 hours of initiating therapy with and following dosage increases of ULTRACET.
To reduce the risk of respiratory depression, proper dosing and titration of ULTRACET are essential
[see
Dosage and Administration (2)]
. Overestimating the ULTRACET dosage when converting patients from another opioid product can result in a fatal overdose with the first dose.
Accidental ingestion of even one dose of ULTRACET, especially by children, can result in respiratory depression and death due to an overdose of tramadol.
Educate patients and caregivers on how to recognize respiratory depression and emphasize the importance of calling 911 or getting emergency medical help right away in the event of a known or suspected overdose
[see
Patient Counseling Information (17)].
Opioids can cause sleep-related breathing disorders including central sleep apnea (CSA) and sleep-related hypoxemia. Opioid use increases the risk of CSA in a dose-dependent fashion. In patients who present with CSA, consider decreasing the opioid dosage using best practices for opioid taper
[see
Dosage and Administration (2.5)]
.
Patient Access to Naloxone for the Emergency Treatment of Opioid Overdose
Discuss the availability of naloxone for the emergency treatment of opioid overdose with the patient and caregiver and assess the potential need for access to naloxone, both when initiating and renewing treatment with ULTRACET. Inform patients and caregivers about the various ways to obtain naloxone as permitted by individual state naloxone dispensing and prescribing requirements or guidelines (e.g., by prescription, directly from a pharmacist, or as part of a community-based program). Educate patients and caregivers on how to recognize respiratory depression and emphasize the importance of calling 911 or getting emergency medical help, even if naloxone is administered
[see
Patient Counseling Information (17)]
.
Consider prescribing naloxone, based on the patient’s risk factors for overdose, such as concomitant use of CNS depressants, a history of opioid use disorder, or prior opioid overdose. However, the presence of risk factors for overdose should not prevent the proper management of pain in any given patient. Also consider prescribing naloxone if the patient has household members (including children) or other close contacts at risk for accidental exposure or overdose. If naloxone is prescribed, educate patients and caregivers on how to treat with naloxone.
[see
Warnings and Precautions (5.1,
5.8),
Patient Counseling Information (17)]
.
5.4 Ultra-Rapid Metabolism of Tramadol and Other Risk Factors for Life-threatening Respiratory Depression in Children
Life-threatening respiratory depression and death have occurred in children who received tramadol. Tramadol and codeine are subject to variability in metabolism based upon CYP2D6 genotype (described below), which can lead to increased exposure to an active metabolite. Based upon postmarketing reports with tramadol or with codeine, children younger than 12 years of age may be more susceptible to the respiratory depressant effects of tramadol. Furthermore, children with obstructive sleep apnea who are treated with opioids for post-tonsillectomy and/or adenoidectomy pain may be particularly sensitive to their respiratory depressant effect. Because of the risk of life-threatening respiratory depression and death:
- ULTRACET is contraindicated for all children younger than 12 years of age
[see
Contraindications (4)]
.
- ULTRACET is contraindicated for postoperative management in pediatric patients younger than 18 years of age following tonsillectomy and/or adenoidectomy
[see
Contraindications (4)]
.
- Avoid the use of ULTRACET in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of tramadol unless the benefits outweigh the risks. Risk factors include conditions associated with hypoventilation such as postoperative status, obstructive sleep apnea, obesity, severe pulmonary disease, neuromuscular disease, and concomitant use of other medications that cause respiratory depression.
- As with adults, when prescribing opioids for adolescents, healthcare providers should choose the lowest effective dose for the shortest period of time and inform patients and caregivers about these risks and the signs of opioid overdose
[see
Use in Specific Populations (8.4),
Overdosage (10)]
.
Nursing Mothers
Tramadol is subject to the same polymorphic metabolism as codeine, with ultra-rapid metabolizers of CYP2D6 substrates being potentially exposed to life-threatening levels of
O-desmethyltramadol (M1). At least one death was reported in a nursing infant who was exposed to high levels of morphine in breast milk because the mother was an ultra-rapid metabolizer of codeine. A baby nursing from an ultra-rapid metabolizer mother taking ULTRACET could potentially be exposed to high levels of M1, and experience life-threatening respiratory depression. For this reason, breastfeeding is not recommended during treatment with ULTRACET
[see
Use in Specific Populations (8.2)]
.
CYP2D6 Genetic Variability: Ultra-rapid metabolizer
Some individuals may be ultra-rapid metabolizers because of a specific CYP2D6 genotype (gene duplications denoted as *1/*1×N or *1/*2×N). The prevalence of this CYP2D6 phenotype varies widely and has been estimated at 1 to 10% for Whites (European, North American), 3 to 4% for Blacks (African Americans), 1 to 2% for East Asians (Chinese, Japanese, Korean), and may be greater than 10% in certain racial/ethnic groups (i.e., Oceanian, Northern African, Middle Eastern, Ashkenazi Jews, Puerto Rican). These individuals convert tramadol into its active metabolite,
O-desmethyltramadol (M1), more rapidly and completely than other people. This rapid conversion results in higher than expected serum M1 levels. Even at labeled dosage regimens, individuals who are ultra-rapid metabolizers may have life-threatening or fatal respiratory depression or experience signs of overdose (such as extreme sleepiness, confusion, or shallow breathing)
[see
Overdosage (10)]
. Therefore, individuals who are ultra-rapid metabolizers should not use ULTRACET.
5.5 Neonatal Opioid Withdrawal Syndrome
Prolonged use of ULTRACET during pregnancy can result in withdrawal in the neonate. Neonatal opioid withdrawal syndrome, unlike opioid withdrawal syndrome in adults, may be life-threatening if not recognized and treated, and requires management according to protocols developed by neonatology experts. Observe newborns for signs of neonatal opioid withdrawal syndrome and manage accordingly. Advise pregnant women using opioids for a prolonged period of the risk of neonatal opioid withdrawal syndrome and ensure that appropriate treatment will be available
[see
Use in Specific Populations (8.1) and
Patient Counseling Information (17)].
5.6 Risks of Interactions with Drugs Affecting Cytochrome P450 Isoenzymes
The effects of concomitant use or discontinuation of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors on levels of tramadol and M1 from ULTRACET are complex. Use of cytochrome P450 3A4 inducers, 3A4 inhibitors, or 2D6 inhibitors with ULTRACET requires careful consideration of the effects on the parent drug, tramadol, which is a weak serotonin and norepinephrine reuptake inhibitor and µ-opioid agonist, and the active metabolite, M1, which is more potent than tramadol in µ-opioid receptor binding
[see
Drug Interactions (7)]
.
Risks of Concomitant Use or Discontinuation of Cytochrome P450 2D6 Inhibitors
The concomitant use of ULTRACET with all cytochrome P450 2D6 inhibitors (e.g., amiodarone, quinidine) may result in an increase in tramadol plasma levels and a decrease in the levels of the active metabolite, M1. A decrease in M1 exposure in patients who have developed physical dependence to tramadol, may result in signs and symptoms of opioid withdrawal and reduced efficacy. The effect of increased tramadol levels may be an increased risk for serious adverse events including seizures and serotonin syndrome.
Discontinuation of a concomitantly used cytochrome P450 2D6 inhibitor may result in a decrease in tramadol plasma levels and an increase in active metabolite M1 levels, which could increase or prolong adverse reactions related to opioid toxicity and may cause potentially fatal respiratory depression.
Follow patients receiving ULTRACET and any CYP2D6 inhibitor for the risk of serious adverse events including seizures and serotonin syndrome, signs and symptoms that may reflect opioid toxicity, and opioid withdrawal when ULTRACET is used in conjunction with inhibitors of CYP2D6
[see
Drug Interactions (7)]
.
Cytochrome P450 3A4 Interaction
The concomitant use of ULTRACET with cytochrome P450 3A4 inhibitors, such as macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), and protease inhibitors (e.g., ritonavir) or discontinuation of a cytochrome P450 3A4 inducer such as rifampin, carbamazepine, and phenytoin, may result in an increase in tramadol plasma concentrations, which could increase or prolong adverse reactions, increase the risk for serious adverse events including seizures and serotonin syndrome, and may cause potentially fatal respiratory depression.
The concomitant use of ULTRACET with all cytochrome P450 3A4 inducers or discontinuation of a cytochrome P450 3A4 inhibitor may result in lower tramadol levels. This may be associated with a decrease in efficacy, and in some patients, may result in signs and symptoms of opioid withdrawal.
Follow patients receiving ULTRACET and any CYP3A4 inhibitor or inducer for the risk for serious adverse events including seizures and serotonin syndrome, signs and symptoms that may reflect opioid toxicity and opioid withdrawal when ULTRACET is used in conjunction with inhibitors and inducers of CYP3A4
[see
Drug Interactions (7)]
.
5.7 Hepatotoxicity
ULTRACET contains tramadol hydrochloride and acetaminophen. Acetaminophen has been associated with cases of acute liver failure, at times resulting in liver transplant and death. Most of the cases of liver injury are associated with the use of acetaminophen at doses that exceed 4,000 milligrams per day, and often involve more than one acetaminophen-containing product. The excessive intake of acetaminophen may be intentional to cause self-harm or unintentional as patients attempt to obtain more pain relief or unknowingly take other acetaminophen-containing products.
The risk of acute liver failure is higher in individuals with underlying liver disease and in individuals who ingest alcohol while taking acetaminophen.
Instruct patients to look for acetaminophen or APAP on package labels and not to use more than one product that contains acetaminophen. Instruct patients to seek medical attention immediately upon ingestion of more than 4,000 milligrams of acetaminophen per day, even if they feel well.
5.8 Risks from Concomitant Use with Benzodiazepines or Other CNS Depressants
Profound sedation, respiratory depression, coma, and death may result from the concomitant use of ULTRACET with benzodiazepines or other CNS depressants (e.g., non-benzodiazepine sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, other opioids, alcohol). Because of these risks, reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate.
Observational studies have demonstrated that concomitant use of opioid analgesics and benzodiazepines increases the risk of drug-related mortality compared to use of opioid analgesics alone. Because of similar pharmacological properties, it is reasonable to expect similar risk with the concomitant use of other CNS depressant drugs with opioid analgesics
[see
Drug Interactions (7)]
.
If the decision is made to prescribe a benzodiazepine or other CNS depressant concomitantly with an opioid analgesic, prescribe the lowest effective dosages and minimum durations of concomitant use. In patients already receiving an opioid analgesic, prescribe a lower initial dose of the benzodiazepine or other CNS depressant than indicated in the absence of an opioid, and titrate based on clinical response. If an opioid analgesic is initiated in a patient already taking a benzodiazepine or other CNS depressant, prescribe a lower initial dose of the opioid analgesic, and titrate based on clinical response. Follow patients closely for signs and symptoms of respiratory depression and sedation.
If concomitant use is warranted, consider prescribing naloxone for the emergency treatment of opioid overdose
[see
Dosage and Administration (2.2),
Warnings and Precautions (5.3)]
.
Advise both patients and caregivers about the risks of respiratory depression and sedation when ULTRACET is used with benzodiazepines or other CNS depressants (including alcohol and illicit drugs). Advise patients not to drive or operate heavy machinery until the effects of concomitant use of the benzodiazepine or other CNS depressant have been determined. Screen patients for risk of substance use disorders, including opioid abuse and misuse, and warn them of the risk for overdose and death associated with the use of additional CNS depressants including alcohol and illicit drugs
[see
Drug Interactions (7),
Patient Counseling Information (17)]
.
5.9 Serotonin Syndrome Risk
Cases of serotonin syndrome, a potentially life-threatening condition, have been reported with the use of tramadol, including ULTRACET, during concomitant use with serotonergic drugs.
Serotonergic drugs include selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that affect the serotonergic neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), and drugs that impair metabolism of serotonin (including MAO inhibitors, both those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue)
[see
Drug Interactions (7)].
This may occur within the recommended dosage range.
Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, coma), autonomic instability (e.g., tachycardia, labile blood pressure, hyperthermia), neuromuscular aberrations (e.g., hyperreflexia, incoordination, rigidity), and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea). The onset of symptoms generally occurs within several hours to a few days of concomitant use, but may occur later than that. Discontinue ULTRACET if serotonin syndrome is suspected.
5.10 Increased Risk of Seizures
Seizures have been reported in patients receiving tramadol within the recommended dosage range. Spontaneous postmarketing reports indicate that seizure risk is increased with doses of tramadol above the recommended range.
Concomitant use of tramadol increases the seizure risk in patients taking:
[see
Drug Interactions (7)]
.
- Selective serotonin re-uptake inhibitors (SSRIs) and Serotonin-norepinephrine re-uptake inhibitors (SNRIs) antidepressants or anorectics,
- Tricyclic antidepressants (TCAs), and other tricyclic compounds (e.g., cyclobenzaprine, promethazine, etc.),
- Other opioids,
- MAO inhibitors
[see
Warnings and Precautions (5.9),
Drug Interactions (7)]
- Neuroleptics, or
- Other drugs that reduce the seizure threshold.
Risk of seizures may also increase in patients with epilepsy, those with a history of seizures, or in patients with a recognized risk for seizure (such as head trauma, metabolic disorders, alcohol and drug withdrawal, CNS infections).
In tramadol overdose, naloxone administration may increase the risk of seizure.
5.11 Suicide Risk
- Do not prescribe ULTRACET for patients who are suicidal or addiction-prone. Consideration should be given to the use of non-narcotic analgesics in patients who are suicidal or depressed
[see
Drug Abuse and Dependence (9)].
- Prescribe ULTRACET with caution for patients with a history of misuse and/or are currently taking CNS-active drugs including tranquilizers, or antidepressant drugs, or alcohol in excess, and patients who suffer from emotional disturbance or depression
[see
Drug Interactions (7)]
.
- Inform patients not to exceed the recommended dose and to limit their intake of alcohol
[see
Dosage and Administration (2),
Warnings and Precautions (5.7,
5.8)]
.
5.12 Adrenal Insufficiency
Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use. Presentation of adrenal insufficiency may include non-specific symptoms and signs including nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. If adrenal insufficiency is suspected, confirm the diagnosis with diagnostic testing as soon as possible. If adrenal insufficiency is diagnosed, treat with physiologic replacement doses of corticosteroids. Wean the patient off of the opioid to allow adrenal function to recover and continue corticosteroid treatment until adrenal function recovers. Other opioids may be tried as some cases reported use of a different opioid without recurrence of adrenal insufficiency. The information available does not identify any particular opioids as being more likely to be associated with adrenal insufficiency.
5.13 Life-Threatening Respiratory Depression in Patients with Chronic Pulmonary Disease or in Elderly, Cachectic, or Debilitated Patients
The use of ULTRACET in patients with acute or severe bronchial asthma in an unmonitored setting or in the absence of resuscitative equipment is contraindicated
[see
Contraindications (4)]
.
Patients with Chronic Pulmonary Disease: ULTRACET-treated patients with significant chronic obstructive pulmonary disease or cor pulmonale, and those with a substantially decreased respiratory reserve, hypoxia, hypercapnia, or pre-existing respiratory depression are at increased risk of decreased respiratory drive including apnea, even at recommended dosages of ULTRACET
[see
Warnings and Precautions (5.3)]
.
Elderly, Cachectic, or Debilitated Patients: Life-threatening respiratory depression is more likely to occur in elderly, cachectic, or debilitated patients because they may have altered pharmacokinetics, or altered clearance, compared to younger, healthier patients
[see
Warnings and Precautions (5.3)]
.
Monitor such patients closely, particularly when initiating and titrating ULTRACET and when ULTRACET is given concomitantly with other drugs that depress respiration
[see
Warnings and Precautions (5.8),
Drug Interactions (7)]
. Alternatively, consider the use of non-opioid analgesics in these patients.
5.14 Severe Hypotension
ULTRACET may cause severe hypotension including orthostatic hypotension and syncope in ambulatory patients. There is increased risk in patients whose ability to maintain blood pressure has already been compromised by a reduced blood volume or concurrent administration of certain CNS depressant drugs (e.g., phenothiazines or general anesthetics)
[see
Drug Interactions (7)]
. Monitor these patients for signs of hypotension after initiating or titrating the dosage of ULTRACET. In patients with circulatory shock, ULTRACET may cause vasodilation that can further reduce cardiac output and blood pressure. Avoid the use of ULTRACET in patients with circulatory shock.
5.15 Risk of Use in Patients with Increased Intracranial Pressure, Brain Tumors, Head Injury, or Impaired Consciousness
In patients who may be susceptible to the intracranial effects of CO
2 retention (e.g., those with evidence of increased intracranial pressure or brain tumors), ULTRACET may reduce respiratory drive, and the resultant CO
2 retention can further increase intracranial pressure. Monitor such patients for signs of sedation and respiratory depression, particularly when initiating therapy with ULTRACET.
Opioids may also obscure the clinical course in a patient with a head injury. Avoid the use of ULTRACET in patients with impaired consciousness or coma.
5.16 Serious Skin Reactions
Rarely, acetaminophen may cause serious skin reactions such as acute generalized exanthematous pustulosis (AGEP), Stevens-Johnson Syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal. Patients should be informed about the signs of serious skin reactions, and use of the drug should be discontinued at the first appearance of skin rash or any other sign of hypersensitivity.
5.17 Risk of Use in Patients with Gastrointestinal Conditions
ULTRACET is contraindicated in patients with known or suspected gastrointestinal obstruction, including paralytic ileus
[see
Contraindications (4)]
.
The tramadol in ULTRACET may cause spasm of the sphincter of Oddi. Opioids may cause increases in serum amylase. Monitor patients with biliary tract disease, including acute pancreatitis, for worsening symptoms.
5.18 Anaphylaxis and Other Hypersensitivity Reactions
Serious and rarely fatal anaphylactic reactions have been reported in patients receiving therapy with tramadol. When these events do occur it is often following the first dose. Other reported allergic reactions include pruritus, hives, bronchospasm, angioedema, toxic epidermal necrolysis, and Stevens-Johnson syndrome. Patients with a history of anaphylactoid reactions to tramadol and other opioids may be at increased risk and therefore should not receive ULTRACET. If anaphylaxis or other hypersensitivity occurs, stop administration of ULTRACET immediately, discontinue ULTRACET permanently, and do not rechallenge with any formulation of tramadol. Advise patients to seek immediate medical attention if they experience any symptoms of a hypersensitivity reaction
[see
Contraindications (4)].
There have been postmarketing reports of hypersensitivity and anaphylaxis associated with the use of acetaminophen. Clinical signs included swelling of the face, mouth, and throat, respiratory distress, urticaria, rash, pruritus, and vomiting. There were infrequent reports of life-threatening anaphylaxis requiring emergency medical attention. Instruct patients to discontinue ULTRACET immediately and seek medical care if they experience these symptoms. Do not prescribe ULTRACET for patients with acetaminophen allergy.
5.19 Increased Risk of Hepatotoxicity with Concomitant Use of Other Acetaminophen-containing Products
Due to the potential for acetaminophen hepatotoxicity at doses higher than the recommended dose, ULTRACET should not be used concomitantly with other acetaminophen containing products.
5.20 Withdrawal
Do not abruptly discontinue ULTRACET in a patient physically dependent on opioids. When discontinuing ULTRACET in a physically dependent patient, gradually taper the dosage. Rapid tapering of tramadol and acetaminophen in a patient physically dependent on opioids may lead to a withdrawal syndrome and return of pain
[see
Dosage and Administration (2.5),
Drug Abuse and Dependence (9.3)]
.
Additionally, avoid the use of mixed agonist/antagonist (e.g., pentazocine, nalbuphine, and butorphanol) or partial agonist (e.g., buprenorphine) analgesics in patients who are receiving a full opioid agonist analgesic, including ULTRACET. In these patients, mixed agonist/antagonist and partial agonist analgesics may reduce the analgesic effect and/or may precipitate withdrawal symptoms
[see
Drug Interactions (7)]
.
5.21 Driving and Operating Machinery
ULTRACET may impair the mental or physical abilities needed to perform potentially hazardous activities such as driving a car or operating machinery. Warn patients not to drive or operate dangerous machinery unless they are tolerant to the effects of ULTRACET and know how they will react to the medication
[see
Patient Counseling Information (17)]
.
5.22 Hyponatremia
Hyponatremia (serum sodium < 135 mmol/L) has been reported with the use of tramadol, and many cases are severe (sodium level < 120 mmol/L). Most cases of hyponatremia occurred in females over the age of 65 and within the first week of therapy. In some reports, hyponatremia resulted from the syndrome of inappropriate antidiuretic hormone secretion (SIADH). Monitor for signs and symptoms of hyponatremia (e.g., confusion, disorientation), during treatment with ULTRACET, especially during initiation of therapy. If signs and symptoms of hyponatremia are present, initiate appropriate treatment (e.g., fluid restriction) and discontinue ULTRACET
[see
Dosage and Administration: Safe Reduction or Discontinuation of ULTRACET (2.5)].
5.23 Hypoglycemia
Cases of tramadol-associated hypoglycemia have been reported, some resulting in hospitalization. In most cases, patients had predisposing risk factors (e.g. diabetes). If hypoglycemia is suspected, monitor blood glucose levels and consider drug discontinuation as appropriate
[see
Dosage and Administration: Safe Reduction or Discontinuation of ULTRACET (2.5)].
6. Adverse Reactions/Side Effects
The following serious adverse reactions are discussed, or described in greater detail, in other sections:
- Addiction, Abuse, and Misuse
[see
Warnings and Precautions (5.1)]
- Life-Threatening Respiratory Depression
[see
Warnings and Precautions (5.3)]
- Ultra-Rapid Metabolism of Tramadol and Other Risk Factors for Life-threatening Respiratory Depression in Children
[see
Warnings and Precautions (5.4)]
- Neonatal Opioid Withdrawal Syndrome
[see
Warnings and Precautions (5.5)]
- Hepatotoxicity
[see
Warnings and Precautions (5.7)]
- Interactions with Benzodiazepines or Other CNS Depressants
[see
Warnings and Precautions (5.8)]
- Serotonin Syndrome
[see
Warnings and Precautions (5.9)]
- Seizures
[see
Warnings and Precautions (5.10)]
- Suicide
[see
Warnings and Precautions (5.11)]
- Adrenal Insufficiency
[see
Warnings and Precautions (5.12)]
- Severe Hypotension
[see
Warnings and Precautions (5.14)]
- Gastrointestinal Adverse Reactions
[see
Warnings and Precautions (5.17)]
- Hypersensitivity Reactions
[see
Warnings and Precautions (5.18)]
- Withdrawal
[see
Warnings and Precautions (5.20)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The most common incidence of treatment-emergent adverse events (≥3.0%) in subjects from clinical trials was constipation, diarrhea, nausea, somnolence, anorexia, dizziness, and sweating increased.
Table 1 shows the incidence rate of treatment-emergent adverse events reported in ≥2.0% of subjects over five days of ULTRACET use in clinical trials (subjects took an average of at least 6 tablets per day).
| Body System
Preferred Term |
ULTRACET (N=142)
(%) |
|---|---|
|
|
| Gastrointestinal System Disorders | |
| Constipation | 6 |
| Diarrhea | 3 |
| Nausea | 3 |
| Dry Mouth | 2 |
| Psychiatric Disorders | |
| Somnolence | 6 |
| Anorexia | 3 |
| Insomnia | 2 |
| Central & Peripheral Nervous System | |
| Dizziness | 3 |
| Skin and Appendages | |
| Sweating Increased | 4 |
| Pruritus | 2 |
| Reproductive Disorders, Male
* |
|
| Prostatic Disorder | 2 |
Incidence at least 1%, causal relationship at least possible or greater:
The following lists adverse reactions that occurred with an incidence of at least 1% in single-dose or repeated-dose clinical trials of ULTRACET.
Body as a Whole – Asthenia, fatigue, hot flushes
Central and Peripheral Nervous System – Dizziness, headache, tremor
Gastrointestinal System – Abdominal pain, constipation, diarrhea, dyspepsia, flatulence, dry mouth, nausea, vomiting
Psychiatric Disorders – Anorexia, anxiety, confusion, euphoria, insomnia, nervousness, somnolence
Skin and Appendages – Pruritus, rash, increased sweating
Selected Adverse events occurring at less than 1%:
The following lists clinically relevant adverse reactions that occurred with an incidence of less than 1% in ULTRACET clinical trials.
Body as a Whole – Chest pain, rigors, syncope, withdrawal syndrome
Cardiovascular Disorders – Hypertension, aggravated hypertension, hypotension
Central and Peripheral Nervous System – Ataxia, convulsions, hypertonia, migraine, aggravated migraine, involuntary muscle contractions, paresthesias, stupor, vertigo
Gastrointestinal System – Dysphagia, melena, tongue edema
Hearing and Vestibular Disorders – Tinnitus
Heart Rate and Rhythm Disorders – Arrhythmia, palpitation, tachycardia
Liver and Biliary System – Hepatic function abnormal
Metabolic and Nutritional Disorders – Weight decrease
Psychiatric Disorders – Amnesia, depersonalization, depression, drug abuse, emotional lability, hallucination, impotence, paroniria, abnormal thinking
Red Blood Cell Disorders – Anemia
Respiratory System – Dyspnea
Urinary System – Albuminuria, micturition disorder, oliguria, urinary retention
Vision Disorders – Abnormal vision
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of tramadol-containing products. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Serotonin syndrome: Cases of serotonin syndrome, a potentially life-threatening condition, have been reported during concomitant use of opioids with serotonergic drugs.
Adrenal insufficiency: Cases of adrenal insufficiency have been reported with opioid use, more often following greater than one month of use.
Anaphylaxis: Anaphylaxis has been reported with ingredients contained in ULTRACET.
Androgen deficiency: Cases of androgen deficiency have occurred with chronic use of opioids
[see
Clinical Pharmacology (12.2)]
.
QT prolongation/torsade de pointes: Cases of QT prolongation and/or
torsade de pointes have been reported with tramadol use. Many of these cases were reported in patients taking another drug labeled for QT prolongation, in patients with a risk factor for QT prolongation (e.g., hypokalemia), or in the overdose setting.
Eye disorders – miosis, mydriasis
Metabolism and nutrition disorders – Hyponatremia: Cases of severe hyponatremia and/or SIADH have been reported in patients taking tramadol, most often in females over the age of 65, and within the first week of therapy
[see
Warnings and Precautions (5.22)].
Hypoglycemia: Cases of hypoglycemia have been reported in patients taking tramadol. Most reports were in patients with predisposing risk factors, including diabetes or renal insufficiency, or in elderly patients
[see
Warnings and Precautions (5.23)].
Nervous system disorders – movement disorder, speech disorder
Psychiatric disorders – delirium
Other clinically significant adverse experiences previously reported with tramadol hydrochloride:
Other events which have been reported with the use of tramadol products and for which a causal association has not been determined include: vasodilation, orthostatic hypotension, myocardial ischemia, pulmonary edema, allergic reactions (including anaphylaxis and urticaria, Stevens-Johnson syndrome/TENS), cognitive dysfunction, difficulty concentrating, depression, suicidal tendency, hepatitis, liver failure, and gastrointestinal bleeding. Reported laboratory abnormalities included elevated creatinine and liver function tests. Serotonin syndrome (whose symptoms may include mental status change, hyperreflexia, fever, shivering, tremor, agitation, diaphoresis, seizures, and coma) has been reported with tramadol when used concomitantly with other serotonergic agents such as SSRIs and MAOIs.
7. Drug Interactions
Table 2 includes clinically significant interactions with ULTRACET.
| Inhibitors of CYP2D6 | |
| Clinical Impact: | The concomitant use of ULTRACET and CYP2D6 inhibitors may result in an increase in the plasma concentration of tramadol and a decrease in the plasma concentration of M1, particularly when an inhibitor is added after a stable dose of ULTRACET is achieved. Since M1 is a more potent µ-opioid agonist, decreased M1 exposure could result in decreased therapeutic effects, and may result in signs and symptoms of opioid withdrawal in patients who had developed physical dependence to tramadol. Increased tramadol exposure can result in increased or prolonged therapeutic effects and increased risk for serious adverse events including seizures and serotonin syndrome.
After stopping a CYP2D6 inhibitor, as the effects of the inhibitor decline, the tramadol plasma concentration will decrease and the M1 plasma concentration will increase which could increase or prolong therapeutic effects but also increase adverse reactions related to opioid toxicity, and may cause potentially fatal respiratory depression [see Clinical Pharmacology (12.3)] . |
| Intervention: | If concomitant use of a CYP2D6 inhibitor is necessary, follow patients closely for adverse reactions including opioid withdrawal, seizures and serotonin syndrome.
If a CYP2D6 inhibitor is discontinued, consider lowering ULTRACET dosage until stable drug effects are achieved. Follow patients closely for adverse events including respiratory depression and sedation. |
| Examples: | Quinidine, fluoxetine, paroxetine and bupropion |
| Inhibitors of CYP3A4 | |
| Clinical Impact: | The concomitant use of ULTRACET and CYP3A4 inhibitors can increase the plasma concentration of tramadol and may result in a greater amount of metabolism via CYP2D6 and greater levels of M1. Follow patients closely for increased risk of serious adverse events including seizures and serotonin syndrome, and adverse reactions related to opioid toxicity including potentially fatal respiratory depression, particularly when an inhibitor is added after a stable dose of ULTRACET is achieved.
After stopping a CYP3A4 inhibitor, as the effects of the inhibitor decline, the tramadol plasma concentration will decrease [see Clinical Pharmacology (12.3)] , resulting in decreased opioid efficacy and possibly signs and symptoms of opioid withdrawal in patients who had developed physical dependence to tramadol. |
| Intervention: | If concomitant use is necessary, consider dosage reduction of ULTRACET until stable drug effects are achieved. Follow patients closely for seizures and serotonin syndrome, and signs of respiratory depression and sedation at frequent intervals.
If a CYP3A4 inhibitor is discontinued, consider increasing the ULTRACET dosage until stable drug effects are achieved and follow patients for signs and symptoms of opioid withdrawal. |
| Examples: | Macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g. ketoconazole), protease inhibitors (e.g., ritonavir) |
| CYP3A4 Inducers | |
| Clinical Impact: | The concomitant use of ULTRACET and CYP3A4 inducers can decrease the plasma concentration of tramadol
[see Clinical Pharmacology (12.3)] , resulting in decreased efficacy or onset of a withdrawal syndrome in patients who have developed physical dependence to tramadol. After stopping a CYP3A4 inducer, as the effects of the inducer decline, the tramadol plasma concentration will increase [see Clinical Pharmacology (12.3)] , which could increase or prolong both the therapeutic effects and adverse reactions, and may cause serious respiratory depression, seizures and serotonin syndrome. |
| Intervention: | If concomitant use is necessary, consider increasing the ULTRACET dosage until stable drug effects are achieved. Follow patients for signs of opioid withdrawal.
If a CYP3A4 inducer is discontinued, consider ULTRACET dosage reduction and monitor for seizures and serotonin syndrome, and signs of sedation and respiratory depression. Patients taking carbamazepine, a CYP3A4 inducer, may have a significantly reduced analgesic effect of tramadol. Because carbamazepine increases tramadol metabolism and because of the seizure risk associated with tramadol, concomitant administration of ULTRACET and carbamazepine is not recommended. |
| Examples: | Rifampin, carbamazepine, phenytoin |
| Benzodiazepines and Other Central Nervous System (CNS) Depressants | |
| Clinical Impact: | Due to additive pharmacologic effect, the concomitant use of benzodiazepines or other CNS depressants, including alcohol, can increase the risk of hypotension, respiratory depression, profound sedation, coma, and death. |
| Intervention: | Reserve concomitant prescribing of these drugs for use in patients for whom alternative treatment options are inadequate. Limit dosages and durations to the minimum required. Follow patients closely for signs of respiratory depression and sedation
[see Warnings and Precautions (5.8)] . If concomitant use is warranted, consider prescribing naloxone for the emergency treatment of opioid overdose [see Dosage and Administration (2.2), Warnings and Precautions (5.1, 5.3, 5.8)] . |
| Examples: | Benzodiazepines and other sedatives/hypnotics, anxiolytics, tranquilizers, muscle relaxants, general anesthetics, antipsychotics, other opioids, alcohol. |
| Serotonergic Drugs | |
| Clinical Impact: | The concomitant use of opioids with other drugs that affect the serotonergic neurotransmitter system has resulted in serotonin syndrome. |
| Intervention: | If concomitant use is warranted, carefully observe the patient, particularly during treatment initiation and dose adjustment. Discontinue ULTRACET if serotonin syndrome is suspected. |
| Examples: | Selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), tricyclic antidepressants (TCAs), triptans, 5-HT3 receptor antagonists, drugs that affect the serotonin neurotransmitter system (e.g., mirtazapine, trazodone, tramadol), certain muscle relaxants (i.e., cyclobenzaprine, metaxalone), monoamine oxidase (MAO) inhibitors (those intended to treat psychiatric disorders and also others, such as linezolid and intravenous methylene blue). |
| Monoamine Oxidase Inhibitors (MAOIs) | |
| Clinical Impact: | MAOI interactions with opioids may manifest as serotonin syndrome
[see Warnings and Precautions (5.9)] or opioid toxicity (e.g., respiratory depression, coma) [see Warnings and Precautions (5.3)] . |
| Intervention: | Do not use ULTRACET in patients taking MAOIs or within 14 days of stopping such treatment. |
| Examples: | phenelzine, tranylcypromine, linezolid |
| Mixed Agonist/Antagonist and Partial Agonist Opioid Analgesics | |
| Clinical Impact: | May reduce the analgesic effect of ULTRACET and/or precipitate withdrawal symptoms. |
| Intervention: | Avoid concomitant use. |
| Examples: | butorphanol, nalbuphine, pentazocine, buprenorphine |
| Muscle Relaxants | |
| Clinical Impact: | Tramadol may enhance the neuromuscular blocking action of skeletal muscle relaxants and produce an increased degree of respiratory depression. |
| Intervention: | Monitor patients for signs of respiratory depression that may be greater than otherwise expected and decrease the dosage of ULTRACET and/or the muscle relaxant as necessary. Due to the risk of respiratory depression with concomitant use of skeletal muscle relaxants and opioids, consider prescribing naloxone for the emergency treatment of opioid overdose
[see Dosage and Administration (2.2), Warnings and Precautions (5.3, 5.8)] . |
| Diuretics | |
| Clinical Impact: | Opioids can reduce the efficacy of diuretics by inducing the release of antidiuretic hormone. |
| Intervention: | Monitor patients for signs of diminished diuresis and/or effects on blood pressure and increase the dosage of the diuretic as needed. |
| Anticholinergic Drugs | |
| Clinical Impact: | The concomitant use of anticholinergic drugs may increase risk of urinary retention and/or severe constipation, which may lead to paralytic ileus. |
| Intervention: | Monitor patients for signs of urinary retention or reduced gastric motility when ULTRACET is used concomitantly with anticholinergic drugs. |
| Digoxin | |
| Clinical Impact: | Postmarketing surveillance of tramadol has revealed rare reports of digoxin toxicity. |
| Intervention: | Follow patients for signs of digoxin toxicity and adjust dosage of digoxin as needed. |
| Warfarin | |
| Clinical Impact: | Postmarketing surveillance of tramadol has revealed rare reports of alteration of warfarin effect, including elevation of prothrombin times. |
| Intervention: | Monitor the prothrombin time of patients on warfarin for signs of an interaction and adjust the dosage of warfarin as needed. |
8. Use In Specific Populations
8.1 Pregnancy
Risk Summary
Prolonged use of opioid analgesics during pregnancy may cause neonatal opioid withdrawal syndrome
[see
Warnings and Precautions (5.5)]
. Available data with ULTRACET in pregnant women are insufficient to inform a drug-associated risk for major birth defects and miscarriage.
In animal reproduction studies, the combination of tramadol and acetaminophen decreased fetal weights and increased supernumerary ribs at 1.6 times the maximum recommended human daily dosage (MRHD). In separate animal reproduction studies, tramadol administration alone during organogenesis decreased fetal weights and reduced ossification in mice, rats, and rabbits at 1.4, 0.6, and 3.6 times the maximum recommended human daily dosage (MRHD). Tramadol decreased pup body weight and increased pup mortality at 1.2 and 1.9 times the MRHD.
Reproductive and developmental studies in rats and mice from the published literature identified adverse events at clinically relevant doses with acetaminophen. Treatment of pregnant rats with doses of acetaminophen approximately 1.3 times the maximum human daily dose (MRHD) showed evidence of fetotoxicity and increases in bone variations in the fetuses. In another study, necrosis was observed in the liver and kidney of both pregnant rats and fetuses at doses approximately 1.9 times the MHDD. In mice treated with acetaminophen at doses within the clinical dosing range, cumulative adverse effects on reproduction were seen in a continuous breeding study. A reduction in number of litters of the parental mating pair was observed as well as retarded growth and abnormal sperm in their offspring and reduced birth weight in the next generation
[see
Data]
. Based on animal data, advise pregnant women of the potential risk to a fetus.
All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2–4% and 15–20%, respectively.
Clinical Considerations
Fetal/Neonatal Adverse Reactions
Prolonged use of opioid analgesics during pregnancy for medical or nonmedical purposes can result in respiratory depression and physical dependence in the neonate and neonatal opioid withdrawal syndrome shortly after birth.
Neonatal opioid withdrawal syndrome presents as irritability, hyperactivity and abnormal sleep pattern, high pitched cry, tremor, vomiting, diarrhea and failure to gain weight. The onset, duration, and severity of neonatal opioid withdrawal syndrome vary based on the specific opioid used, duration of use, timing and amount of last maternal use, and rate of elimination of the drug by the newborn. Observe newborns for symptoms and signs of neonatal opioid withdrawal syndrome and manage accordingly
[see
Warnings and Precautions (5.5)]
.
Neonatal seizures, neonatal withdrawal syndrome, fetal death and stillbirth have been reported with tramadol hydrochloride during postmarketing.
Labor or Delivery
ULTRACET is not recommended for use in pregnant women during or immediately prior to labor, when other analgesic techniques are more appropriate. Opioids cross the placenta and may produce respiratory depression and psycho-physiologic effects in neonates. An opioid antagonist, such as naloxone, must be available for reversal of opioid induced respiratory depression in the neonate. ULTRACET is not recommended for use in pregnant women during or immediately prior to labor, when other analgesic techniques are more appropriate. Opioid analgesics, including ULTRACET, can prolong labor through actions which temporarily reduce the strength, duration, and frequency of uterine contractions. However, this effect is not consistent and may be offset by an increased rate of cervical dilation, which tends to shorten labor. Monitor neonates exposed to opioid analgesics during labor for signs of excess sedation and respiratory depression.
Tramadol has been shown to cross the placenta. The mean ratio of serum tramadol in the umbilical veins compared to maternal veins was 0.83 for 40 women given tramadol during labor.
The effect of ULTRACET, if any, on the later growth, development, and functional maturation of the child is unknown.
Data
Animal Data
No drug-related teratogenic effects were observed in the progeny of rats treated orally with tramadol and acetaminophen. The tramadol/acetaminophen combination product was shown to be embryotoxic and fetotoxic in rats at a maternally toxic dose, 50/434 mg/kg tramadol/acetaminophen (1.6 times the maximum daily human tramadol/acetaminophen dosage), but was not teratogenic at this dose level. Embryo and fetal toxicity consisted of decreased fetal weights and increased supernumerary ribs. Tramadol has been shown to be embryotoxic and fetotoxic in mice, (120 mg/kg), rats (25 mg/kg) and rabbits (75 mg/kg) at maternally toxic dosages, but was not teratogenic at these dose levels. These doses on a mg/m
2 basis are 1.9, 0.8, and 4.9 times the maximum recommended human daily dosage (MRHD) for mouse, rat and rabbit, respectively.
No drug-related teratogenic effects were observed in progeny of mice (up to 140 mg/kg), rats (up to 80 mg/kg) or rabbits (up to 300 mg/kg) treated with tramadol by various routes. Embryo and fetal toxicity consisted primarily of decreased fetal weights, skeletal ossification and increased supernumerary ribs at maternally toxic dose levels. Transient delays in developmental or behavioral parameters were also seen in pups from rat dams allowed to deliver. Embryo and fetal lethality were reported only in one rabbit study at 300 mg/kg, a dose that would cause extreme maternal toxicity in the rabbit. The dosages listed for mouse, rat and rabbit are 2.3, 2.6, and 19 times the MRHD, respectively.
Tramadol alone was evaluated in peri- and post-natal studies in rats. Progeny of dams receiving oral (gavage) dose levels of 50 mg/kg (300 mg/m
2 or 1.6 times the maximum daily human tramadol dosage) or greater had decreased weights, and pup survival was decreased early in lactation at 80 mg/kg (480 mg/m
2 or 2.6 times the maximum daily human tramadol dosage).
Studies in pregnant rats that received oral acetaminophen during organogenesis at doses up to 1.3 times the maximum human daily dose (MHDD = 2.6 grams/day, based on a body surface area comparison) showed evidence of fetotoxicity (reduced fetal weight and length) and a dose-related increase in bone variations (reduced ossification and rudimentary rib changes). Offspring had no evidence of external, visceral, or skeletal malformations.
When pregnant rats received oral acetaminophen throughout gestation at doses of 1.9-times the MHDD (based on a body surface area comparison), areas of necrosis occurred in both the liver and kidney of pregnant rats and fetuses. These effects did not occur in animals that received oral acetaminophen at doses 0.5-times the MHDD, based on a body surface area comparison.
In a continuous breeding study, pregnant mice received 0.25, 0.5, or 1.0% acetaminophen via the diet (357, 715, or 1430 mg/kg/day). These doses are approximately 0.7, 1.3, and 2.7 times the MHDD, respectively, based on a body surface area comparison. A dose-related reduction in body weights of fourth and fifth litter offspring of the treated mating pair occurred during lactation and post-weaning at all doses. Animals in the high dose group had a reduced number of litters per mating pair, male offspring with an increased percentage of abnormal sperm, and reduced birth weights in the next generation pups.
8.2 Lactation
Risk Summary
ULTRACET is not recommended for obstetrical preoperative medication or for post-delivery analgesia in nursing mothers because its safety in infants and newborns has not been studied.
Tramadol and its metabolite,
O-desmethyltramadol (M1), are present in human milk. There is no information on the effects of the drug on the breastfed infant or the effects of the drug on milk production. The M1 metabolite is more potent than tramadol in mu opioid receptor binding
[see
Clinical Pharmacology (12.1)].
Published studies have reported tramadol and M1 in colostrum with administration of tramadol to nursing mothers in the early post-partum period. Women who are ultra-rapid metabolizers of tramadol may have higher than expected serum levels of M1, potentially leading to higher levels of M1 in breast milk that can be dangerous in their breastfed infants. In women with normal tramadol metabolism, the amount of tramadol secreted into human milk is low and dose-dependent. Because of the potential for serious adverse reactions, including excess sedation and respiratory depression in a breastfed infant, advise patients that breastfeeding is not recommended during treatment with ULTRACET.
Clinical Considerations
If infants are exposed to ULTRACET through breast milk, they should be monitored for excess sedation and respiratory depression. Withdrawal symptoms can occur in breastfed infants when maternal administration of an opioid analgesic is stopped, or when breast-feeding is stopped.
Data
Following a single IV 100 mg dose of tramadol, the cumulative excretion in breast milk within 16 hours post dose was 100 mcg of tramadol (0.1% of the maternal dose) and 27 mcg of M1.
8.3 Females and Males of Reproductive Potential
Infertility
Chronic use of opioids may cause reduced fertility in females and males of reproductive potential. It is not known whether these effects on fertility are reversible
[see
Adverse Reactions (6.2),
Clinical Pharmacology (12.2),
Nonclinical Toxicology (13.1)]
.
8.4 Pediatric Use
The safety and effectiveness of ULTRACET in pediatric patients have not been established.
Life-threatening respiratory depression and death have occurred in children who received tramadol
[see
Warnings and Precautions (5.4)]
. In some of the reported cases, these events followed tonsillectomy and/or adenoidectomy, and one of the children had evidence of being an ultra-rapid metabolizer of tramadol (i.e., multiple copies of the gene for cytochrome P450 isoenzyme 2D6). Children with sleep apnea may be particularly sensitive to the respiratory depressant effects of tramadol.
Because of the risk of life-threatening respiratory depression and death:
- ULTRACET is contraindicated for all children younger than age 12 years of age
[see
Contraindications (4)]
.
- ULTRACET is contraindicated for postoperative management in pediatric patients younger than 18 years of age following tonsillectomy and/or adenoidectomy
[see
Contraindications (4)]
.
- Avoid the use of ULTRACET in adolescents 12 to 18 years of age who have other risk factors that may increase their sensitivity to the respiratory depressant effects of tramadol unless the benefits outweigh the risks. Risk factors include conditions associated with hypoventilation such as postoperative status, obstructive sleep apnea, obesity, severe pulmonary disease, neuromuscular disease, and concomitant use of other medications that cause respiratory depression.
8.5 Geriatric Use
Elderly patients (65 years of age or older) may have increased sensitivity to tramadol. In general, use caution when selecting a dosage for an elderly patient, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
Respiratory depression is the chief risk for elderly patients treated with opioids, and has occurred after large initial doses were administered to patients who were not opioid-tolerant or when opioids were co-administered with other agents that depress respiration. Titrate the dosage of ULTRACET slowly in geriatric patients and monitor closely for signs of central nervous system and respiratory depression
[see
Warnings and Precautions (5.3)].
Tramadol and acetaminophen are known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function.
8.6 Hepatic Impairment
The pharmacokinetics and tolerability of ULTRACET in patients with impaired hepatic function have not been studied. Based on information using tramadol immediate-release tablets in subjects with advanced cirrhosis of the liver, tramadol exposure was higher and half-lives of tramadol and active metabolite M1 were longer than in subjects with normal hepatic function
[see
Clinical Pharmacology (12.3)].
As tramadol and acetaminophen are both extensively metabolized by the liver, the use of ULTRACET in patients with hepatic impairment is not recommended
[see
Warnings and Precautions (5.7)]
.
8.7 Renal Impairment
The pharmacokinetics and tolerability of ULTRACET in patients with renal impairment has not been studied. Based on studies using tramadol extended-release tablets, the excretion of tramadol and metabolite M1 is reduced in patients with creatinine clearance of less than 30 mL/min. In patients with creatinine clearances of less than 30 mL/min, it is recommended that the dosage of ULTRACET not exceed 2 tablets every 12 hours.
[see
Dosage and Administration (2.3)]
. The total amount of tramadol and M1 removed during a 4 hour dialysis period is less than 7% of the administered dose based on studies using tramadol alone. Monitor closely for signs of respiratory depression, sedation, and hypotension.
8.8 Sex
Tramadol clearance was 20% higher in female subjects compared to males in four Phase 1 studies of ULTRACET in 50 male and 34 female healthy subjects. The clinical significance of this difference is unknown.
9. Drug Abuse and Dependence
9.1 Controlled Substance
ULTRACET contains tramadol, a Schedule IV controlled substance.
9.2 Abuse
ULTRACET contains tramadol, a substance with a high potential for abuse similar to other opioids and can be abused and is subject to misuse, addiction, and criminal diversion
[see
Warnings and Precautions (5.1)]
.
All patients treated with opioids require careful monitoring for signs of abuse and addiction, since use of opioid analgesic products carries the risk of addiction even under appropriate medical use.
Prescription drug abuse is the intentional non-therapeutic use of a prescription drug, even once, for its rewarding psychological or physiological effects.
Drug addiction is a cluster of behavioral, cognitive, and physiological phenomena that develop after repeated substance use and includes: a strong desire to take the drug, difficulties in controlling its use, persisting in its use despite harmful, or potentially harmful, consequences, a higher priority given to drug use than to other activities and obligations, increased tolerance, and sometimes a physical withdrawal.
«Drug seeking» behavior is very common in persons with substance use disorders. Drug seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing or referral, repeated «loss» of prescriptions, tampering with prescriptions, and reluctance to provide prior medical records or contact information for other treating physician(s). «Doctor shopping» (visiting multiple prescribers) to obtain additional prescriptions is common among drug abusers and people suffering from untreated addiction. Preoccupation with achieving adequate pain relief can be appropriate behavior in a patient with poor pain control.
Abuse and addiction are separate and distinct from physical dependence and tolerance. Healthcare providers should be aware that addiction may not be accompanied by concurrent tolerance and symptoms of physical dependence in all addicts. In addition, abuse of opioids can occur in the absence of true addiction.
ULTRACET, like other opioids, can be diverted for non-medical use into illicit channels of distribution. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests, as required by state and federal law, is strongly advised.
Proper assessment of the patient, proper prescribing practices, periodic re-evaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
Risks Specific to Abuse of ULTRACET
ULTRACET is for oral use only. Abuse of ULTRACET poses a risk of overdose and death. The risk is increased with concurrent abuse of ULTRACET with alcohol and other central nervous system depressants.
Parenteral drug abuse is commonly associated with transmission of infectious diseases such as hepatitis and HIV.
9.3 Dependence
Both tolerance and physical dependence can develop during chronic opioid therapy. Tolerance is the need for increasing doses of opioids to maintain a defined effect such as analgesia (in the absence of disease progression or other external factors). Tolerance may occur to both the desired and undesired effects of drugs, and may develop at different rates for different effects.
Physical dependence is a physiological state in which the body adapts to the drug after a period of regular exposure, resulting in withdrawal symptoms after abrupt discontinuation or a significant dosage reduction of a drug. Withdrawal also may be precipitated through the administration of drugs with opioid antagonist activity (e.g., naloxone, nalmefene), mixed agonist/antagonist analgesics (e.g., pentazocine, butorphanol, nalbuphine), or partial agonists (e.g., buprenorphine). Physical dependence may not occur to a clinically significant degree until after several days to weeks of continued opioid usage.
Do not abruptly discontinue ULTRACET in a patient physically dependent on opioids. Rapid tapering of ULTRACET in a patient physically dependent on opioids may lead to serious withdrawal symptoms, uncontrolled pain and suicide.
Rapid discontinuation has also been associated with attempts to find other sources of opioid analgesics, which may be confused with drug-seeking for abuse.
When discontinuing opioids, gradually taper the dosage using a patient-specific plan that considers the following: the dose of the opioid the patient has been taking, the duration of treatment, and the physical and psychological attributes of the patient. To improve the likelihood of a successful taper and minimize withdrawal symptoms, it is important that the opioid tapering schedule is agreed upon by the patient. In patients taking opioids for a long duration at high doses, ensure that a multimodal approach to pain management, including mental health support (if needed), is in place prior to initiating an opioid analgesic taper
[see
Dosage and Administration (2.5),
Warnings and Precautions (5.20)].
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal signs
[see
Use in Specific Populations (8.1)]
.
10. Overdosage
Clinical Presentation
ULTRACET is a combination drug. The clinical presentation of overdose may include the signs and symptoms of tramadol toxicity, acetaminophen toxicity or both. The initial symptoms of tramadol overdosage may include respiratory depression and/or seizures. The initial symptoms seen within the first 24 hours following an acetaminophen overdose are: anorexia, nausea, vomiting, malaise, pallor and diaphoresis.
Tramadol
Acute overdosage with tramadol can be manifested by respiratory depression, somnolence progressing to stupor or coma, skeletal muscle flaccidity, cold and clammy skin, constricted pupils, and, in some cases, pulmonary edema, bradycardia, QT prolongation, hypotension, partial or complete airway obstruction, atypical snoring, seizures, and death. Marked mydriasis rather than miosis may be seen with hypoxia in overdose situations.
Deaths due to overdose have been reported with abuse and misuse of tramadol
[see
Warnings and Precautions (5.1)]
. Review of case reports has indicated that the risk of fatal overdose is further increased when tramadol is abused concurrently with alcohol or other CNS depressants, including other opioids.
Acetaminophen
In acute acetaminophen overdosage, dose-dependent, potentially fatal hepatic necrosis is the most serious adverse effect. Renal tubular necrosis, hypoglycemic coma, and thrombocytopenia also occur. Plasma acetaminophen levels >300 mcg/mL at 4 hours after oral ingestion were associated with hepatic damage in 90% of patients; minimal hepatic damage is anticipated if plasma levels at 4 hours are <150 mcg/mL or <37.5 mcg/mL at 12 hours after ingestion. Early symptoms following a potentially hepatotoxic overdose may include: nausea, vomiting, diaphoresis, and general malaise. Clinical and laboratory evidence of hepatic toxicity may not be apparent until 48 to 72 hours post-ingestion.
Treatment of Overdose
A single or multiple drug overdose with tramadol and acetaminophen is a potentially lethal polydrug overdose. Immediate treatment includes support of cardiorespiratory function and measures to reduce drug absorption. Oxygen, intravenous fluids, vasopressors, assisted ventilation, and other supportive measures should be employed as indicated. Because strategies for the management of overdose are continually evolving, it is advisable to contact a poison control center (where available) to determine the latest recommendations for the management of an overdose.
Tramadol
In case of overdose, priorities are the re-establishment of a patent and protected airway and institution of assisted or controlled ventilation, if needed. Employ other supportive measures (including oxygen and vasopressors) in the management of circulatory shock and pulmonary edema as indicated. Cardiac arrest or arrhythmias will require advanced life-support techniques.
Opioid antagonists, such as naloxone, are specific antidotes to respiratory depression resulting from opioid overdose.
For clinically significant respiratory or circulatory depression secondary to opioid overdose, administer an opioid antagonist.
While naloxone will reverse some, but not all, symptoms caused by overdosage with tramadol, the risk of seizures is also increased with naloxone administration. In animals, convulsions following the administration of toxic doses of ULTRACET could be suppressed with barbiturates or benzodiazepines but were increased with naloxone. Naloxone administration did not change the lethality of an overdose in mice. Hemodialysis is not expected to be helpful in an overdose because it removes less than 7% of the administered dose in a 4-hour dialysis period.
Because the duration of opioid reversal is expected to be less than the duration of action of tramadol in ULTRACET, carefully monitor the patient until spontaneous respiration is reliably re-established. If the response to an opioid antagonist is suboptimal or only brief in nature, administer additional antagonist as directed by the product’s prescribing information.
In an individual physically dependent on opioids, administration of the recommended usual dosage of the antagonist will precipitate an acute withdrawal syndrome. The severity of the withdrawal symptoms experienced will depend on the degree of physical dependence and the dose of the antagonist administered. If a decision is made to treat serious respiratory depression in the physically dependent patient, administration of the antagonist should be begun with care and by titration with smaller than usual doses of the antagonist.
Acetaminophen
If an acetaminophen overdose is suspected, obtain a serum acetaminophen assay as soon as possible, but no sooner than 4 hours following oral ingestion. Obtain liver function studies initially and repeat at 24-hour intervals. Administer the antidote N-acetylcysteine (NAC) as early as possible. As a guide to treatment of acute ingestion, the acetaminophen level can be plotted against time since oral ingestion on a nomogram Rumack-Matthew). The lower toxic line on the nomogram is equivalent to 150 mcg/mL at 4 hours and 37.5 mcg/mL at 12 hours. If serum level is above the lower line, administer the entire course of NAC treatment. Withhold NAC therapy if the acetaminophen level is below the lower line.
Serum acetaminophen levels should be obtained immediately if the patient presents 4 hours or more after ingestion to assess potential risk of hepatotoxicity; acetaminophen levels drawn less than 4 hours post-ingestion may be misleading. To obtain the best possible outcome, NAC should be administered as soon as possible where impending or evolving liver injury is suspected. Intravenous NAC may be administered when circumstances preclude oral administration.
Vigorous supportive therapy is required in severe intoxication. Procedures to limit the continuing absorption of the drug must be readily performed since the hepatic injury is dose-dependent and occurs early in the course of intoxication.
11. Ultracet Description
ULTRACET
® (tramadol hydrochloride/acetaminophen) Tablets combines two analgesics, tramadol hydrochloride and opioid agonist, and acetaminophen.
The chemical name for tramadol hydrochloride is (±)cis-2-[(dimethylamino)methyl]-1-(3-methoxyphenyl) cyclohexanol hydrochloride. Its structural formula is:
The molecular weight of tramadol hydrochloride is 299.84. Tramadol hydrochloride is a white, bitter, crystalline, and odorless powder.
The chemical name for acetaminophen is N-acetyl-p-aminophenol. Its structural formula is:
The molecular weight of acetaminophen is 151.17. Acetaminophen is an analgesic and antipyretic agent which occurs as a white, odorless, crystalline powder, possessing a slightly bitter taste.
ULTRACET tablets contain 37.5 mg of tramadol hydrochloride and 325 mg acetaminophen and are light yellow in color. Inactive ingredients in the tablet are carnauba wax, corn starch, hypromellose, iron oxide, magnesium stearate, polyethylene glycol, polysorbate 80, powdered cellulose, pregelatinized corn starch, sodium starch glycolate, and titanium dioxide.
Meets USP Dissolution Test 2.
12. Ultracet — Clinical Pharmacology
The following information is based on studies of tramadol alone or acetaminophen alone, except where otherwise noted:
12.1 Mechanism of Action
ULTRACET contains tramadol, an opioid agonist and inhibitor of norepinephrine and serotonin re-uptake, and acetaminophen. Although the mode of action of tramadol is not completely understood, the analgesic effect of tramadol is believed to be due to both binding to µ-opioid receptors and weak inhibition of reuptake of norepinephrine and serotonin.
Opioid activity of tramadol is due to both low affinity binding of the parent compound and higher affinity binding of the
O-demethylated metabolite M1 to µ-opioid receptors. In animal models, M1 is up to 6 times more potent than tramadol in producing analgesia and 200 times more potent in µ-opioid binding. Tramadol-induced analgesia is only partially antagonized by the opiate antagonist naloxone in several animal tests. The relative contribution of both tramadol and M1 to human analgesia is dependent upon the plasma concentrations of each compound
[see
Clinical Pharmacology (12.3)]
.
Tramadol has been shown to inhibit reuptake of norepinephrine and serotonin
in vitro, as have some other opioid analgesics. These mechanisms may contribute independently to the overall analgesic profile of tramadol.
Acetaminophen is a non-opioid, non-salicylate analgesic. The site and mechanism for the analgesic effect of acetaminophen has not been determined but is thought to primarily involve central actions.
12.2 Pharmacodynamics
Effects on the Central Nervous System
Tramadol produces respiratory depression by direct action on brain stem respiratory centers. The respiratory depression involves a reduction in the responsiveness of the brain stem respiratory centers to both increases in carbon dioxide tension and electrical stimulation.
Tramadol causes miosis, even in total darkness. Pinpoint pupils are a sign of opioid overdose but are not pathognomonic (e.g., pontine lesions of hemorrhagic or ischemic origins may produce similar findings). Marked mydriasis rather than miosis may be seen due to hypoxia in overdose situations.
Effects on the Gastrointestinal Tract and Other Smooth Muscle
Tramadol causes a reduction in motility associated with an increase in smooth muscle tone in the antrum of the stomach and duodenum. Digestion of food in the small intestine is delayed and propulsive contractions are decreased. Propulsive peristaltic waves in the colon are decreased, while tone may be increased to the point of spasm resulting in constipation. Other opioid-induced effects may include a reduction in biliary and pancreatic secretions, spasm of sphincter of Oddi, and transient elevations in serum amylase.
Effects on the Cardiovascular System
Tramadol produces peripheral vasodilation which may result in orthostatic hypotension or syncope. Manifestations of histamine release and/or peripheral vasodilation may include pruritus, flushing, red eyes, sweating, and/or orthostatic hypotension.
The effect of oral tramadol on the QTcF interval was evaluated in a double-blind, randomized, four-way crossover, placebo- and positive- (moxifloxacin) controlled study in 68 adult male and female healthy subjects. At a 600 mg/day dose (1.5-fold the maximum immediate-release daily dose), the study demonstrated no significant effect on the QTcF interval.
Effects on the Endocrine System
Opioids inhibit the secretion of adrenocorticotropic hormone (ACTH), cortisol, and luteinizing hormone (LH) in humans
[see
Warnings and Precautions (5.12),
Adverse Reactions (6.2)]
. They also stimulate prolactin, growth hormone (GH) secretion, and pancreatic secretion of insulin and glucagon.
Chronic use of opioids may influence the hypothalamic-pituitary-gonadal axis, leading to androgen deficiency that may manifest as low libido, impotence, erectile dysfunction, amenorrhea, or infertility. The causal role of opioids in the clinical syndrome of hypogonadism is unknown because the various medical, physical, lifestyle, and psychological stressors that may influence gonadal hormone levels have not been adequately controlled for in studies conducted to date
[see
Adverse Reactions (6.2)]
.
Effects on the Immune System
Opioids have been shown to have a variety of effects on components of the immune system in
in vitro and animal models. The clinical significance of these findings is unknown. Overall, the effects of opioids appear to be modestly immunosuppressive.
Concentration–Efficacy Relationships
The minimum effective analgesic concentration will vary widely among patients, especially among patients who have been previously treated with potent opioid agonists. The minimum effective analgesic concentration of tramadol for any individual patient may increase over time due to an increase in pain, the development of a new pain syndrome and/or the development of analgesic tolerance
[see
Dosage and Administration (2.1)]
.
Concentration–Adverse Reaction Relationships
There is a relationship between increasing tramadol plasma concentration and increasing frequency of dose-related opioid adverse reactions such as nausea, vomiting, CNS effects, and respiratory depression. In opioid-tolerant patients, the situation may be altered by the development of tolerance to opioid-related adverse reactions
[see
Dosage and Administration (2.1,
2.3)]
.
12.3 Pharmacokinetics
Tramadol is administered as a racemate and both the [-] and [+] forms of both tramadol and M1 are detected in the circulation.
Absorption
The absolute bioavailability of tramadol from ULTRACET tablets has not been determined. Tramadol has a mean absolute bioavailability of approximately 75% following administration of a single 100 mg oral dose of ULTRAM tablets. The mean peak plasma concentration of racemic tramadol and M1 after administration of two ULTRACET tablets occurs at approximately two and three hours, respectively, post-dose.
The pharmacokinetics of plasma tramadol and acetaminophen following oral administration of one ULTRACET tablet are shown in Table 3. Tramadol has a slower absorption and longer half-life when compared to acetaminophen.
| Parameter
* |
(+)-Tramadol | (-)-Tramadol | (+)-M1 | (-)-M1 | acetaminophen | |||||
|---|---|---|---|---|---|---|---|---|---|---|
|
||||||||||
| C
max (ng/mL) |
64.3 | (9.3) | 55.5 | (8.1) | 10.9 | (5.7) | 12.8 | (4.2) | 4.2 | (0.8) |
| t
max (h) |
1.8 | (0.6) | 1.8 | (0.7) | 2.1 | (0.7) | 2.2 | (0.7) | 0.9 | (0.7) |
| CL/F (mL/min) | 588 | (226) | 736 | (244) | — | — | — | — | 365 | (84) |
| t
1/2 (h) |
5.1 | (1.4) | 4.7 | (1.2) | 7.8 | (3.0) | 6.2 | (1.6) | 2.5 | (0.6) |
A single-dose pharmacokinetic study of ULTRACET in volunteers showed no drug interactions between tramadol and acetaminophen.
Upon multiple oral dosing to steady state, however, the bioavailability of tramadol and metabolite M1 was lower for the combination tablets compared to tramadol administered alone. The decrease in AUC was 14% for (+)-tramadol, 10.4% for (-)-tramadol, 11.9% for (+)-M1, and 24.2% for (-)-M1. The cause of this reduced bioavailability is not clear.
Peak plasma concentrations of acetaminophen occur within one hour and are not affected by co-administration with tramadol. Following single- or multiple-dose administration of ULTRACET, no significant change in acetaminophen pharmacokinetics was observed when compared to acetaminophen given alone.
Food Effect
When ULTRACET was administered with food, the time to peak plasma concentration was delayed for approximately 35 minutes for tramadol and almost one hour for acetaminophen. However, peak plasma concentrations, and the extents of absorption, of tramadol and acetaminophen were not affected. The clinical significance of this difference is unknown.
Distribution
The volume of distribution of tramadol was 2.6 and 2.9 L/kg in male and female subjects, respectively, following a 100 mg intravenous dose. The binding of tramadol to human plasma proteins is approximately 20% and binding also appears to be independent of concentration up to 10 mcg/mL. Saturation of plasma protein binding occurs only at concentrations outside the clinically relevant range.
Acetaminophen appears to be widely distributed throughout most body tissues except fat. Its apparent volume of distribution is about 0.9 L/kg. A relatively small portion (~20%) of acetaminophen is bound to plasma protein.
Elimination
Tramadol is eliminated primarily through metabolism by the liver and the metabolites are eliminated primarily by the kidneys. The mean (SD) apparent total clearance of tramadol after a single 37.5 mg dose is 588 (226) mL/min for the (+) isomer and 736 (244) mL/min for the (-) isomer. The plasma elimination half-lives of racemic tramadol and M1 are approximately 5–6 and 7 hours, respectively, after administration of ULTRACET. The apparent plasma elimination half-life of racemic tramadol increased to 7–9 hours upon multiple dosing of ULTRACET.
The half-life of acetaminophen is about 2 to 3 hours in adults. It is somewhat shorter in children and somewhat longer in neonates and in cirrhotic patients. Acetaminophen is eliminated from the body primarily by formation of glucuronide and sulfate conjugates in a dose dependent manner.
Metabolism
Following oral administration, tramadol is extensively metabolized by a number of pathways, including CYP2D6 and CYP3A4, as well as by conjugation of parent and metabolites. The major metabolic pathways appear to be
N— and
O-demethylation and glucuronidation or sulfation in the liver. Metabolite M1 (
O-desmethyltramadol) is pharmacologically active in animal models. Formation of M1 is dependent on CYP2D6 and as such is subject to inhibition, which may affect the therapeutic response
[see
Drug Interactions (7)]
.
Approximately 7% of the population has reduced activity of the CYP2D6 isoenzyme of cytochrome P450. These individuals are «poor metabolizers» of debrisoquine, dextromethorphan, and tricyclic antidepressants, among other drugs. Based on a population PK analysis of Phase 1 studies in healthy subjects, concentrations of tramadol were approximately 20% higher in «poor metabolizers» versus «extensive metabolizers,» while M1 concentrations were 40% lower.
In vitro drug interaction studies in human liver microsomes indicate that inhibitors of CYP2D6 such as fluoxetine and its metabolite norfluoxetine, amitriptyline, and quinidine inhibit the metabolism of tramadol to various degrees. The full pharmacological impact of these alterations in terms of either efficacy or safety is unknown.
Acetaminophen is primarily metabolized in the liver by first-order kinetics and involves three principal separate pathways:
- conjugation with glucuronide;
- conjugation with sulfate; and
- oxidation via the cytochrome, P450-dependent, mixed-function oxidase enzyme pathway to form a reactive intermediate metabolite, which conjugates with glutathione and is then further metabolized to form cysteine and mercapturic acid conjugates. The principal cytochrome P450 isoenzyme involved appears to be CYP2E1, with CYP1A2 and CYP3A4 as additional pathways.
In adults, the majority of acetaminophen is conjugated with glucuronic acid and, to a lesser extent, with sulfate. These glucuronide-, sulfate-, and glutathione-derived metabolites lack biologic activity. In premature infants, newborns, and young infants, the sulfate conjugate predominates.
Excretion
Approximately 30% of the tramadol dose is excreted in the urine as unchanged drug, whereas 60% of the dose is excreted as metabolites.
Less than 9% of acetaminophen is excreted unchanged in the urine.
Special Populations
Hepatic Impairment
Pharmacokinetics of tramadol was studied in patients with mild or moderate hepatic impairment after receiving multiple doses of tramadol extended-release 100 mg. The exposure of (+)-and (-)-tramadol was similar in mild and moderate hepatic impairment patients in comparison to patients with normal hepatic function. However, exposure of (+)- and (-)-M1 decreased ~50% with increased severity of the hepatic impairment (from normal to mild and moderate). The pharmacokinetics of tramadol after the administration of tramadol extended-release has not been studied in patients with severe hepatic impairment. After the administration of tramadol immediate-release tablets to patients with advanced cirrhosis of the liver, tramadol area under the plasma concentration time curve was larger and the tramadol and M1 half-lives were longer than subjects with normal hepatic function
[see
Use in Specific Populations (8.6)].
Renal Impairment
Impaired renal function results in a decreased rate and extent of excretion of tramadol and its active metabolite, M1. The pharmacokinetics of tramadol were studied in patients with mild or moderate renal impairment after receiving multiple doses of tramadol extended-release 100 mg. There is no consistent trend observed for tramadol exposure related to renal function in patients with mild (CLcr: 50–80 mL/min) or moderate (CLcr: 30–50 mL/min) renal impairment in comparison to patients with normal renal function. However, exposure of M1 increased 20–40% with increased severity of the renal impairment (from normal to mild and moderate). tramadol extended-release has not been studied in patients with severe renal impairment (CLcr <30 mL/min). The total amount of tramadol and M1 removed during a 4-hour dialysis period is less than 7% of the administered dose
[see
Dosage and Administration (2.4),
Use in Specific Populations (8.7)]
.
Geriatric Population
A population pharmacokinetic analysis of data obtained from a clinical trial in patients with chronic pain treated with ULTRACET, which included 55 patients between 65 and 75 years of age and 19 patients over 75 years of age, showed no significant changes in the pharmacokinetics of tramadol and acetaminophen in elderly patients with normal renal and hepatic function
[see
Use in Specific Populations (8.5)]
Sex
Tramadol clearance was 20% higher in female subjects compared to males on four Phase 1 studies of ULTRACET in 50 male and 34 female healthy subjects.
Poor / Extensive Metabolizers, CYP2D6
The formation of the active metabolite, M1, is mediated by CYP2D6. Approximately 7% of the population has reduced activity of the CYP2D6 isoenzyme of cytochrome P-450. These individuals are «poor metabolizers» of debrisoquine, dextromethorphan, and tricyclic antidepressants, among other drugs. Based on a population PK analysis of Phase 1 studies with immediate-release tablets in healthy subjects, concentrations of tramadol were approximately 20% higher in «poor metabolizers» versus «extensive metabolizers,» while M1 concentrations were 40% lower.
Drug Interaction Studies
CYP2D6 Inhibitors
In vitro drug interaction studies in human liver microsomes indicate that inhibitors of CYP2D6 (fluoxetine, norfluoxetine, amitriptyline, and quinidine) inhibit the metabolism of tramadol to various degrees, suggesting that concomitant administration of these compounds could result in increases in tramadol concentrations and decreased concentrations of M1. The full pharmacological impact of these alterations in terms of either efficacy or safety is unknown.
Quinidine
Tramadol is metabolized to M1 by CYP2D6. A study was conducted to examine the effect of quinidine, a selective inhibitor of CYP2D6, on the pharmacokinetics of tramadol by administering 200 mg quinidine two hours before the administration of 100 mg tramadol extended release tablet. The results demonstrated that the exposure of tramadol increased 50–60% and the exposure of M1 decreased 50–60%.
In vitro drug interaction studies in human liver microsomes indicate that tramadol has no effect on quinidine metabolism
[see
Warnings and Precautions (5.6) and
Drug Interactions (7)]
.
Cimetidine
Concomitant administration of tramadol and cimetidine does not result in clinically significant changes in tramadol pharmacokinetics. Therefore, no alteration of the ULTRACET dosage regimen is recommended.
CYP3A4 Inhibitors and Inducers
Tramadol is metabolized by CYP3A4. Administration of CYP3A4 inhibitors, such as ketoconazole and erythromycin, or CYP3A4 inducers, such as rifampin and St. John’s Wort, with tramadol may affect the metabolism of tramadol leading to altered tramadol exposure
[see
Warnings and Precautions (5.3 and
5.6) and
Drug Interactions (7)]
.
Carbamazepine
Carbamazepine, a CYP3A4 inducer, increases tramadol metabolism. Patients taking carbamazepine may have a significantly reduced analgesic effect of tramadol. Concomitant administration of tramadol and carbamazepine is not recommended.
Potential for Tramadol to Affect Other Drugs
In vitro studies indicate that tramadol is unlikely to inhibit the CYP3A4-mediated metabolism of other drugs when tramadol is administered concomitantly at therapeutic doses. Tramadol does not appear to induce its own metabolism in humans, since observed maximal plasma concentrations after multiple oral doses are higher than expected based on single dose data.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
There are no animal or laboratory studies on the combination product (tramadol and acetaminophen) to evaluate carcinogenesis, mutagenesis, or impairment of fertility. Data on the individual components are described below.
Carcinogenesis
A slight but statistically significant increase in two common murine tumors, pulmonary and hepatic, was observed in an NMRI mouse carcinogenicity study, particularly in aged mice. Mice were dosed orally up to 30 mg/kg in the drinking water (0.5 times the maximum recommended daily human dosage or MRHD) for approximately two years, although the study was not done with the Maximum Tolerated Dose. This finding is not believed to suggest risk in humans. No evidence of carcinogenicity was noted in a rat 2-year carcinogenicity study testing oral doses of up to 30 mg/kg in the drinking water (1 times the MRHD).
Long-term studies in mice and rats have been completed by the National Toxicology Program to evaluate the carcinogenic potential of acetaminophen. In 2-year feeding studies, F344/N rats and B6C3F1 mice were fed a diet containing acetaminophen up to 6000 ppm. Female rats demonstrated equivocal evidence of carcinogenic activity based on increased incidences of mononuclear cell leukemia at 1.2 times the maximum human daily dose (MHDD) of 2.6 grams/day, based on a body surface area comparison. In contrast, there was no evidence of carcinogenic activity in male rats (1.1 times) or mice (1.9–2.2 times the MHDD, based on a body surface area comparison).
Mutagenesis
Tramadol was mutagenic in the presence of metabolic activation in the mouse lymphoma assay. Tramadol was not mutagenic in the
in vitro bacterial reverse mutation assay using
Salmonella and
E. coli (Ames), the mouse lymphoma assay in the absence of metabolic activation, the
in vitro chromosomal aberration assay, or the
in vivo micronucleus assay in bone marrow.
Acetaminophen was not mutagenic in the bacterial reverse mutation assay (Ames test). In contrast, acetaminophen tested positive for induction of sister chromatid exchanges and chromosomal aberrations in
in vitro assays using Chinese hamster ovary cells. In the published literature, acetaminophen has been reported to be clastogenic when administered a dose of 1500 mg/kg/day to the rat model (3.6-times the MHDD, based on a body surface area comparison). In contrast, no clastogenicity was noted at a dose of 750 mg/kg/day (2.8-times the MHDD, based on a body surface area comparison), suggesting a threshold effect.
Impairment of Fertility
No effects on fertility were observed for tramadol at oral dose levels up to 50 mg/kg in male rats and 75 mg/kg in female rats. These dosages are 1.6 and 2.4 times the MRHD
[see
Use in Specific Populations (8.3)]
.
In studies of acetaminophen conducted by the National Toxicology Program, fertility assessments have been completed in Swiss mice via a continuous breeding study. There were no effects on fertility parameters in mice consuming up to 1.7 times the MHDD of acetaminophen, based on a body surface area comparison. Although there was no effect on sperm motility or sperm density in the epididymis, there was a significant increase in the percentage of abnormal sperm in mice consuming 1.7 times the MHDD (based on a body surface area comparison) and there was a reduction in the number of mating pairs producing a fifth litter at this dose, suggesting the potential for cumulative toxicity with chronic administration of acetaminophen near the upper limit of daily dosing.
Published studies in rodents report that oral acetaminophen treatment of male animals at doses that are 1.2 times the MHDD and greater (based on a body surface area comparison) result in decreased testicular weights, reduced spermatogenesis, reduced fertility, and reduced implantation sites in females given the same doses. These effects appear to increase with the duration of treatment. The clinical significance of these findings is not known.
14. Clinical Studies
14.1 Single-Dose Studies for Treatment of Acute Pain
In single-dose studies in acute pain, two tablets of ULTRACET administered to patients with pain following oral surgical procedures provided greater relief than placebo or either of the individual components given at the same dose. The onset of pain relief after ULTRACET was faster than tramadol alone. Onset of analgesia occurred in less than one hour. The duration of pain relief after ULTRACET was longer than acetaminophen alone. Analgesia was generally comparable to that of the comparator, ibuprofen.
16. How is Ultracet supplied
ULTRACET
® (tramadol hydrochloride/acetaminophen) tablets containing 37.5 mg tramadol hydrochloride and 325 mg acetaminophen are light yellow, coated, capsule-shaped tablets debossed with «O-M» on one side and «650» on the other and are available as follows:
| 100’s: | NDC 50458-650-60 | Bottles of 100 tablets |
| HUD 100’s: | NDC 50458-650-10 | Packages of 100 unit doses in blister packs, 10 cards of 10 tablets each |
Dispense in a tight container. Store at 20–25°C (68–77°F); excursions permitted to 15–30°C (59–86°F). [see USP Controlled Room Temperature].
Store ULTRACET securely and dispose of properly
[see
Patient Counseling Information (17)].
17. Patient Counseling Information
Advise the patient to read the FDA-approved patient labeling (Medication Guide).
Storage and Disposal
Because of the risks associated with accidental ingestion, misuse, and abuse, advise patients to store ULTRACET securely, out of sight and reach of children, and in a location not accessible by others, including visitors to the home
[see
Warnings and Precautions (5.1,
5.20),
Drug Abuse and Dependence (9.2)]
. Inform patients that leaving ULTRACET unsecured can pose a deadly risk to others in the home.
Advise patients and caregivers that when medicines are no longer needed, they should be disposed of promptly. Inform patients that medicine take-back options are the preferred way to safely dispose of most types of unneeded medicines. If no take back programs or Drug Enforcement Administration (DEA)-registered collectors are available, instruct patients to dispose of ULTRACET by following these four steps:
- Mix ULTRACET (do not crush) with an unpalatable substance such as dirt, cat litter, or used coffee grounds;
- Place the mixture in a container such as a sealed plastic bag;
- Throw the container in the household trash;
- Delete all personal information on the prescription label of the empty bottle.
Inform patients that they can visit www.fda.gov/drugdisposal for additional information on disposal of unused medicines.
Addiction, Abuse, and Misuse
Inform patients that the use of ULTRACET, even when taken as recommended, can result in addiction, abuse, and misuse, which can lead to overdose and death
[see
Warnings and Precautions (5.1)]
. Instruct patients not to share ULTRACET with others and to take steps to protect ULTRACET from theft or misuse.
Life-Threatening Respiratory Depression
Inform patients of the risk of life-threatening respiratory depression, including information that the risk is greatest when starting ULTRACET or when the dosage is increased, and that it can occur even at recommended dosages.
Educate patients and caregivers on how to recognize respiratory depression and emphasize the importance of calling 911 or getting emergency medical help right away in the event of a known or suspected overdose
[see
Warnings and Precautions (5.3)].
Patient Access to Naloxone for the Emergency Treatment of Opioid Overdose
Discuss with the patient and caregiver the availability of naloxone for the emergency treatment of opioid overdose, both when initiating and renewing treatment with ULTRACET. Inform patients and caregivers about the various ways to obtain naloxone as permitted by individual state naloxone dispensing and prescribing requirements or guidelines (e.g., by prescription, directly from a pharmacist, or as part of a community-based program)
[see
Dosage and Administration (2.2),
Warnings and Precautions (5.3)]
.
Educate patients and caregivers on how to recognize the signs and symptoms of an overdose.
Explain to patients and caregivers that naloxone’s effects are temporary, and that they must call 911 or get emergency medical help right away in all cases of known or suspected opioid overdose, even if naloxone is administered
[see
Overdosage (10)].
If naloxone is prescribed, also advise patients and caregivers:
- How to treat with naloxone, in the event of an opioid overdose
- To tell family and friends about their naloxone and to keep it in a place where family and friends can access it in an emergency
- To read the Patient Information (or other educational material) that will come with their naloxone. Emphasize the importance of doing this before an opioid emergency happens, so the patient and caregiver will know what to do.
Accidental Ingestion
Inform patients that accidental ingestion, especially by children, may result in respiratory depression or death
[see
Warnings and Precautions (5.3)]
.
Ultra-Rapid Metabolism of Tramadol and Other Risk Factors for Life-threatening Respiratory Depression in Children
Advise caregivers that ULTRACET is contraindicated in children younger than 12 years of age and in children younger than 18 years of age following tonsillectomy and/or adenoidectomy. Advise caregivers of children 12 to 18 years of age receiving ULTRACET to monitor for signs of respiratory depression
[see
Warnings and Precautions (5.4)]
.
Interactions with Benzodiazepines or Other CNS Depressants
Inform patients and caregivers that potentially fatal additive effects may occur if ULTRACET is used with benzodiazepines or other CNS depressants, including alcohol, and not to use these concomitantly unless supervised by a healthcare provider
[see
Warnings and Precautions (5.8),
Drug Interactions (7)]
.
Serotonin Syndrome
Inform patients that tramadol could cause a rare but potentially life-threatening condition, particularly during concomitant use with serotonergic drugs. Warn patients of the symptoms and signs of serotonin syndrome and to seek medical attention right away if symptoms develop. Instruct patients to inform their healthcare provider if they are taking, or plan to take serotonergic medications
[see
Warnings and Precautions (5.9)]
.
MAOI Interaction
Inform patients not to take ULTRACET while using any drugs that inhibit monoamine oxidase. Patients should not start MAOIs while taking ULTRACET
[see
Drug Interactions (7)]
.
Seizures
Inform patients that ULTRACET may cause seizures with concomitant use of serotonergic agents (including SSRIs, SNRIs, and triptans) or drugs that significantly reduce the metabolic clearance of tramadol
[see
Warnings and Precautions (5.10)]
.
Adrenal Insufficiency
Inform patients that opioids could cause adrenal insufficiency, a potentially life-threatening condition. Adrenal insufficiency may present with non-specific symptoms and signs such as nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure. Advise patients to seek medical attention if they experience a constellation of these symptoms
[see
Warnings and Precautions (5.12)]
.
Important Administration Instructions
Instruct patients how to properly take ULTRACET
[see
Dosage and Administration (2)]
.
- Do not adjust the dose of ULTRACET without consulting with a physician or other healthcare provider.
- Do not take more than 4000 milligrams of acetaminophen per day and to call their healthcare provider if they took more than the recommended dose.
Important Discontinuation Instructions
In order to avoid developing withdrawal symptoms, instruct patients not to discontinue ULTRACET without first discussing a tapering plan with the prescriber
[see
Dosage and Administration (2.5)]
.
Hypotension
Inform patients that ULTRACET may cause orthostatic hypotension and syncope. Instruct patients how to recognize symptoms of low blood pressure and how to reduce the risk of serious consequences should hypotension occur (e.g., sit or lie down, carefully rise from a sitting or lying position)
[see
Warnings and Precautions (5.14)]
.
Anaphylaxis
Inform patients that anaphylaxis have been reported with ingredients contained in ULTRACET. Advise patients how to recognize such a reaction and when to seek medical attention
[see
Contraindications (4),
Warnings and Precautions (5.18),
Adverse Reactions (6)]
.
Pregnancy
Neonatal Opioid Withdrawal Syndrome
Inform female patients of reproductive potential that ULTRACET should not be used for more than 5 days and that prolonged use of opioids such as ULTRACET, during pregnancy can result in neonatal opioid withdrawal syndrome, which may be life-threatening if not recognized and treated. The patient should inform their healthcare provider if they have used opioids at any time during their pregnancy
[see
Warnings and Precautions (5.5) and
Use in Specific Populations (8.1)]
.
Embryo-Fetal Toxicity
Inform female patients of reproductive potential that ULTRACET can cause fetal harm and to inform the healthcare provider of a known or suspected pregnancy
[see
Use in Specific Populations (8.1)]
.
Lactation
Advise women that breastfeeding is not recommended during treatment with ULTRACET
[see
Use in Specific Populations (8.2)]
.
Infertility
Inform patients that chronic use of opioids may cause reduced fertility. It is not known whether these effects on fertility are reversible
[see
Use in Specific Populations (8.3)].
Driving or Operating Heavy Machinery
Inform patients that ULTRACET may impair the ability to perform potentially hazardous activities such as driving a car or operating heavy machinery. Advise patients not to perform such tasks until they know how they will react to the medication
[see
Warnings and Precautions (5.21)]
.
Constipation
Advise patients of the potential for severe constipation, including management instructions and when to seek medical attention
[see
Adverse Reactions (6)]
.
Maximum Daily Acetaminophen Use
Advise patients not to take more than 4,000 milligrams of acetaminophen per day and call their doctor if they have taken more than the recommended dose
[see
Warnings and Precautions (5.7,
5.19)].
Use with Other Acetaminophen-Containing Products
Advise patients not to take ULTRACET in combination with other tramadol or acetaminophen-containing products, including over-the-counter preparations
[see
Warnings and Precautions (5.7, 5.19)].
Manufactured for:
Janssen Pharmaceuticals, Inc.
Titusville, New Jersey, 08560, USA
© 2003 Janssen Pharmaceutical Companies
| This Medication Guide has been approved by the U.S. Food and Drug Administration. | Revised: 02/2023 |
| MEDICATION GUIDE ULTRACET ® [UHL-truh-set]
(tramadol hydrochloride/acetaminophen) Tablets, C— IV |
|
ULTRACET is:
|
|
Important information about ULTRACET:
|
|
Important Information Guiding Use in Pediatric Patients:
|
|
Do not take ULTRACET if you have:
|
|
| Before taking ULTRACET, tell your healthcare provider if you have a history of: | |
|
|
|
|
Tell your healthcare provider if you are:
|
|
When taking ULTRACET:
|
|
While taking ULTRACET DO NOT:
|
|
The possible side effects of ULTRACET:
|
|
Get emergency medical help or call 911 right away if you have:
These are not all the possible side effects of ULTRACET. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. For more information go to dailymed.nlm.nih.gov |
PRINCIPAL DISPLAY PANEL — 37.5 mg/325 mg Tablet Bottle Label
NDC 50458-650-60
ULTRACET®
CIV
(37.5 mg tramadol
HCl/325 mg
acetaminophen
tablets)
Please see the
Medication
Guide provided
by your pharmacist.
Keep out of reach of children.
Rx only
100 tablets
- Use
- How to use
- Dosage
- Precautions
- Side-effects
- Warnings
- Interactions
- Contraindications
Why it’s used
Ultracet Tablet is used for the short-term management of moderate to severe pain. It is a prescription medicine. This medicine works by blocking the reuptake of natural chemicals (norepinephrine and serotonin) which produce pain in the body.
Analgesics
How to use
Read the medicine guide provided by your pharmacist, your doctor, or the medicine company. If you have any questions related to Ultracet, ask your doctor or pharmacist. Use Ultracet Tablet as per the instructions provided by your doctor.
Ultracet Tablet is a pain reliever. Pain relievers work the best if used as soon as you feel any pain. They may not work as well if they are delayed until the pain has worsened.
The typical dose of Ultracet for adults is 75 mg tramadol and 650 mg paracetamol every 4 to 6 hours (not more than tramadol 300 mg and paracetamol 2600 mg per day). The maximum dose for adult patients of Ultracet is 300 mg tramadol and 2600 mg paracetamol per day. This medicine is generally used for a period of 5 days for acute pain. It takes less than one hour for this medicine to start its action. Although this medicine is useful to people, it may sometimes be habit-forming or cause addiction. You may be at higher risk if you have a substance use disorder, such as an addiction to drugs, or have an existing addiction, such as to alcohol. To reduce your risk of addiction, take this medicine as prescribed.
Discuss with your doctor if you develop new or worsening symptoms. Discuss with your doctor if skin rash, swelling of the face, swelling of the neck, difficulty in breathing, low blood pressure, and fainting. If you have any kidney disease, the dose should be adjusted in patients with creatinine clearance less than 30 ml/min. Consult with your doctor before stopping the use of Ultracet.
When stopping this medicine, some patients may experience withdrawal symptoms like nervousness (agitation), insomnia, muscle spasm (hyperkinesia), tremor, stomach and intestinal symptoms, panic attacks, severe anxiety, hallucinations, tinnitus, unusual CNS symptoms, sweating, insomnia, high fever (rigors), pain, nausea, diarrhea, upper respiratory symptoms, involuntary erection (piloerection), severe anxiety, and tingling or prickling sensation. You may need to taper (gradually decrease) the dose of this medicine when stopping.
The safety and effectiveness of using Ultracet Tablet in children has not been established. The safety and effectiveness of Ultracet have not been studied in children below the age 12 years.
Avoid consuming alcohol together with Ultracet.
Medicines may be recommended for uses other than those listed in the medicine guide. You should not use Ultracet Tablet for conditions or symptoms for which it was not prescribed. Do not give Ultracet Tablet to other people, even if they have the same conditions or symptoms that you have. The use of this medicine without the advice of a doctor may cause harm.
Follow storage instructions on the product package if available. Store Ultracet Tablet 25°C (77°F); excursions permitted to 15 – 30°C (59 — 86°F), and away from moisture. Store this medicine away from children and pets.
Get TabletWise Pro
Thousands of Classes to Help You Become a Better You.
How to take Ultracet
The dose and frequency of using Ultracet will depend on the following factors:
- age of the patient
- patient’s health
- the health of the patient’s liver
- response to the medicine
Ultracet Dosage
Dosage for moderate to severe pain
Adult
- Recommended: 75 mg of tramadol and 650 mg of paracetamol every 4 to 6 hours
- Maximum: 300 mg of tramadol and 2600 mg of paracetamol in one day
Children (12 years and older)
- Recommended: 75 mg of tramadol and 650 mg of paracetamol every 6 hours
- Maximum: 300 mg of tramadol and 2600 mg of paracetamol in one day
Minimum Age
12 years
Dosage calculation for children
To calculate the dosage for children please use the weight based dose calculator to calculate the appropriate dosage as per the weight of your child.
Forms
Tablet
Strength: 37.5 mg of tramadol and 325 mg of paracetamol
Film Coated Tablet
Strength: 37.5 mg of tramadol and 325 mg of paracetamol
Special Instructions
Patients with creatinine clearance less than 30 mL/min
The recommended dose of Ultracet in these patients should not exceed 75 mg of tramadol and 650 mg of paracetamol every 12 hours. Take necessary precautions while selecting a dose for the elderly as they are more sensitive to side-effects.
Missed Dose
Avoid taking a double dose to make up for the missed dose and continue with your regular schedule.
Overdose
What to do if you overdose on Ultracet?
If this happens, the patient should contact the doctor immediately. At first, proper breathing and blood flow should be ensured. The blood tests should be performed to monitor the liver function every 24 hours. Then, empty the stomach by irritation causing the patient to vomit. Also, naloxone can be given to treat slow and ineffective breathing and diazepam to control seizures. An oral dose of methionine or an injection of N-acetylcysteine (an antidote of paracetamol) should be given in the vein immediately or within 8 hours. The treatment with oral methionine or an injection of N-acetylcysteine is effective in managing the overdose effect if given within 48 hours of overdose.
Symptoms of an overdose of Ultracet
If you use too much of this medicine, it could lead to dangerous levels of the medicine in your body. In such cases, symptoms of an overdose may include:
- abnormalities of glucose breakdown
- an eating disorder identified by weight loss (anorexia)
- an inflammation of pancreas (pancreatitis)
- brain disease (encephalophathy)
- build-up of acid in the body (metabolic acidosis)
- coma
- consciousness disorders
- constriction of the pupil of the eye (miosis)
- excessive sweating (diaphoresis)
- feeling of discomfort
- irregular heartbeat
- kidney failure
- kidney injury (acute tubular necrosis)
- liver damage
- liver failure
- low blood pressure and oxygen deficiency in the body (heart collapse)
- nausea
- pale color of the skin (pallor)
- respiratory arrest
- seizures
- slow and ineffective breathing
- stomach pain
- vomiting
If you think you have overdosed on Ultracet Tablet, call a poison control center immediately. You can look up the poison control center information from the Poison Center Finder at TabletWise.com.
Precautions while using Ultracet
Before you use Ultracet Tablet, discuss with your doctor if you are allergic to it or its ingredients. Your doctor may prescribe an alternative medicine and update your medical records to record this information.
Before you use Ultracet, tell your doctor of your medical and health history including the following: kidney problems, head injury, emotional disturbances, suicidal attempts or ideation, misuse of alcohol, misuse of tranquilizers, misuse of other CNS-active drugs, allergic reactions to codeine and other opioids, seizures, liver problems, or severe lung problems. The use of Ultracet can be fatal in these patients.
The use of this medicine may change sugar level. The use of Ultracet may cause a decrease in sugar level.
The use of Ultracet Tablet may change liver function test. An increase in the liver function test has been reported with the use of Ultracet.
The use of this medicine may change creatinine level. The use of Ultracet may cause an increase in the creatinine level.
Ultracet Tablet can make you feel sleepy. Be careful when using any machinery, driving a vehicle, or doing any other activity that needs you to be fully alert. The consumption of alcohol with Ultracet Tablet can worsen the sleepiness. Ultracet Tablet may cause rarely seizures in some people. If you perform any activities where a loss of consciousness may cause harm to you (or others), you should discuss with your doctor.
The use of Ultracet Tablet is known to be not safe for use in pregnant women. If you are planning to become pregnant or are currently pregnant, you should discuss with your doctor the potential impact of this medicine on the baby before you start to using it. The use of Ultracet during pregnancy may cause loss of a baby during delivery, seizures to the newborn baby, withdrawal syndrome to the newborn baby, and can be possibly fatal to the baby. The use of Ultracet Tablet is not safe for use in women who are breastfeeding. If you are breastfeeding a baby, discuss with your doctor if you should either discontinue breastfeeding or stop using this medicine while breastfeeding. This medicine may pass into breast milk. It is not known if this medicine is safe for use in women who are conceiving. Consult with your doctor before you use Ultracet Tablet. There is no study regarding the effect of Ultracet on fertility has been reported.
Avoid consuming alcohol together with Ultracet. Drinking alcohol may cause central nervous system depression, and slow and ineffective breathing.
This medicine may cause bleeding in the stomach. Regular use of tobacco and alcohol while using this medicine can increase your risk of bleeding. Discuss this aspect with your doctor if you smoke and drink alcohol regularly.
What precautions should be taken during Pregnancy and Nursing, and administering Ultracet to Children or the Older Adults?
Pregnant Women
Contraindicated or Not Recommended
Warning: The use of Ultracet during pregnancy may cause loss of a baby during delivery, seizures to the newborn baby, withdrawal syndrome to the newborn baby, and can be possibly fatal to the baby.
Breastfeeding
Contraindicated or Not Recommended
Warning: This medicine may pass in to breast milk.
Younger Adults Population
Contraindicated or Not Recommended
Warning: No safety and effectiveness data has been established in the children under the age of 12 years.
Older Adults Population
Possibly safe
Warning: In patients older than 75 years, the elimination period of Ultracet from the body may be increased. Thus, the dosing interval of Ultracet should be increased as per the patient’s requirements in such patients.
Ultracet Side-effects
Rarely, the use of Ultracet Tablet may cause the following side-effects:
- a state of dissatisfaction (dysphoria)
- abnormal thinking
- aggravated migraine
- altered mental processes (cognitive dysfunction)
- black tarry stool (melaena)
- bleeding gums
- blood in the stools
- changes in activity
- changes in appetite
- changes in the way you think (perception)
- chest pain
- chills
- collapse
- constriction of the pupil (miosis)
- decreased urine production
- difficulties or pain on passing urine
- difficulty in erection (impotence)
- difficulty in swallowing
- difficulty in urination
- difficulty while focusing (concentrating)
- dilation of the pupil
- disorders of prostate gland (prostatic disorder)
- drug dependence and abuse
- emotional lability
- fainting
- fatigue
- feeling unreal (depersonalization)
- hives
- hot flush
- increase in blood clotting time (elevation of prothrombin times)
- increased muscle tone (hypertonia)
- insensibility
- insomnia
- loss of body movements
- memory loss (amnesia)
- migraine
- muscle weakness (motor weakness)
- nightmare (paroniria)
- nosebleeds
- overresponsive reflexes (hyperreflexia)
- palpitation
- presence of albumin in urine (albuminuria)
- speech disorders
- spinning sensation (vertigo)
- state of intense excitement (euphoria)
- swelling of tongue
- tingling sensation
- tinnitus
- tremor
- weakness
- weight decrease
- withdrawal syndrome
The following severe side-effects may also occur when using Ultracet Tablet:
-
Symptoms: difficulty in breathing slow and ineffective breathing
-
heart rate disorders
-
stomach and intestinal disorders
-
heart disorders
-
nervous system disorders
Symptoms: convulsions aggravated migraine
-
urinary disorders
Symptoms: inability to completely empty the bladder
-
eye disorders
Symptoms: blurred vision, constriction of the pupil of the eye (miosis) dilation of the pupil of the eye
Your doctor has prescribed this Ultracet because they have judged that the benefits outweigh the risks posed by side-effects. Many people using this medicine do not have serious side-effects. This is not a complete list of possible side-effects for Ultracet.
If you experience side-effects or notice other side-effects not listed above, contact your doctor for medical advice. You may also report side-effects to your local food and drug administration authority. You can look up the drug authority contact information from the Drug Authority Finder at TabletWise.com.
Side-effects and Allergic Reactions of Ultracet by Severity and Frequency
Severe Side-effects
Following are the severe side-effects of this medicine:
- Stevens-Johnson syndrome
- abnormal hepatic function
- aggravated hypertension
- agitation
- agranulocytosis
- allergic reactions
- anemia
- angioneurotic oedema
- anorexia
- arrhythmia
- blood dyscrasias
- bradycardia
- bronchospasm
- coma
- convulsion
- delirium
- depression
- dysphagia
- dyspnoea
- elevated creatinine and liver function tests
- gastrointestinal bleeding
- hallucination
- hepatitis
- hypertension
- hypoglycaemia
- hypoprothrombinemia
- hypotension
- liver failure
- low blood platelet count
- miosis
- mydriasis
- myocardial ischemia
- orthostatic hypotension
- pulmonary edema
- rash
- respiratory depression
- rigors
- serious skin reactions
- serotonin syndrome
- slow heart rate
- suicidal tendency
- tachycardia
- thrombocytopenia
- toxic epidermal necrolysis
- transaminases increased
- urinary retention
- vasodilation
- vision blurred
- wheezing
- worsening of asthma
Mild Allergic Reactions
Following are the symptoms of mild allergic reactions to this medicine:
- fainting
- hives
- itching
- swelling of the mouth and throat
- swelling of the neck and face
Serious Allergic Reactions
Following are the symptoms of serious allergic reactions to this medicine:
- Stevens-Johnson syndrome
- bronchospasm
- difficulty in breathing
- drop of blood pressure
- drug induced severe allergic reaction
- respiratory distress
- skin rash
- swelling due to fluid accumulation
- vomiting
If these allergic symptoms appear, stop using this medicine.
If you experience side-effects or notice other side-effects not listed above, contact your doctor for medical advice. You may also report side-effects to your local food and drug administration authority. You can look up the drug authority contact information from the Drug Authority Finder at TabletWise.com.
Warnings
Patients dependent on opioids
The use of Ultracet as a substitute in patients who are dependent on opioids is not recommended.
Children aged 12 years and older
The children aged 12 years and older are at increased risk while using this medicine. The children are at the risk of overdose if a dose of more than tramadol 300 mg and paracetamol 2600 mg is taken. The recommended dose should not be exceeded in children. They also should not use any other drug containing paracetamol or tramadol.
Withdrawal symptoms
The patients are at increased risk of developing withdrawal symptoms such as insomnia, anxiety, chills with sweating and a high fever (rigors), sweating, nausea, diarrhea, tremors, pain, goosebumps (piloerection), hallucinations, upper respiratory tract symptoms, panic attacks, and tingling sensation when Ultracet is stopped immediately. The withdrawal symptoms can be avoided by prescribing a low dose before stopping Ultracet after prolonged treatment.
Patients under use of local anesthetics
The use of Ultracet during general anesthesia with nitrous oxide and enflurane may enhance recall of events that occurred during surgery. The use of Ultracet during surgical anesthesia is not recommended.
Misuse, abuse and diversion
The drug abusers and drug addicts are at increased risk while using this medicine. Misuse and abuse of Ultracet may lead to criminal activity, overdose and can be possibly fatal to such patients. The doctor should take necessary precautions while prescribing Ultracet.
Patients using central nervous system (CNS) depressants
Patients receiving central nervous system depressants such as alcohol, opioids, anesthetic agents, narcotics, phenothiazines, tranquilizers, or sedative hypnotics are at an increased risk. Such patients may see an increased risk of slow and ineffective breathing. Ultracet should be used with caution and a low dose is recommended in such patients.
Patients consuming alcohol and drugs of abuse
Ultracet may cause an additive effect when used in combination with opioids, alcohol or other illegal drugs that cause central nervous system depression. Avoid the use of alcohol and other medicines containing alcohol.
Patients with increased pressure within the skull or head injury
Such patients may experience carbon dioxide retention, increased cerebrospinal fluid pressure, constriction of the pupil of the eye (miosis) and may hide the presence and extent of a skull disease while using Ultracet. Take necessary precautions while using Ultracet in patients with increased intracranial pressure and head injuries by evaluating their mental health conditions.
Ambulatory patients
The patients that perform excessive physical and mental activities are at increased risk while using Ultracet. Ultracet may diminish the mental or physical abilities of the patient required for the execution of tasks such as operating machines or driving a car. Such patients should take caution while consuming Ultracet.
Patients using other paracetamol-containing products
The patients using other paracetamol-containing products together with Ultracet are at increased risk. Such patients may see an increased risk of liver damage. The use of Ultracet with patients using other products containing paracetamol is not recommended.
Liver damage
The patients with liver disease or who consume alcohol are at increased risk while using this medicine. The incidence of liver damage is high in patients using more than one product containing paracetamol or exceeding a dose of 4000 milligrams of paracetamol per day. Such patients are at increased risk of liver failure and fatal conditions. The patients should not use more than one product that contains paracetamol. One should contact the doctor immediately upon taking a dose exceeding 4000 mg of paracetamol per day.
Risk of occurrence of seizures
The patients taking selective serotonin reuptake inhibitors, tricyclic antidepressants, and other tricyclic compounds (for example, cyclobenzaprine and promethazine), other opioids, MAOIs, neuroleptics and other drugs that reduce the seizure threshold are at increased risk. The risk also increases in patients with seizure disorders, a history of seizures or are susceptible to seizures. The patients are at high risk of seizures while using Ultracet. Use this medicine in patients with seizure disorders only when necessary.
Suicidal risk
The patients with the previous history of emotional distress, suicidal thoughts or attempts or history of using alcohol, tranquilizers, and other central nervous system active drugs are at increased risk. The use of tramadol can be possibly fatal in such patients. Ultracet should not be consumed in patients who are addiction-prone or suicidal. The use of non-narcotic analgesics is recommended in such patients. Use Ultracet with caution in patients taking alcohol, tranquilizers, antidepressants or have emotional distress or depression.
A life-threatening condition (also called as serotonin syndrome)
The patients using serotonergic drugs such as selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), triptans, monoamine oxidase inhibitors (MAOIs), tricyclic antidepressants (TCAs) are at increased risk. Also, the patients using drugs which disturbs the metabolism of serotonin or tramadol (for example, CYP2D6 and CYP3A4 inhibitors) are at increased risk while using Ultracet. The patients are at increased risk of developing serotonin syndrome with symptoms like nervousness (agitation), hallucinations, increased heartbeat, coma, increased body temperature, blood pressure changes, lack of coordination (incoordination), overresponsiveness (hyperreflexia), vomiting, diarrhea, and nausea.
Slow and ineffective breathing
The use of Ultracet with anesthetics or alcohol may cause slow and ineffective breathing in the patients. Ultracet should be used with caution in patients who are at risk of slow and ineffective breathing.
Interactions with Ultracet
When two or more medicines are taken together, it can change how the medicines work and increase the risk of side-effects. In medical terms, this is called as a Drug Interaction.
Your doctor’s guidelines may need to be followed while taking this medicine along with quinidine, which is used to treat or prevent irregular heartbeat. The use of quinidine with tramadol may increase the level of tramadol and lowers the level of the amount of metabolite of Ultracet.
Ultracet Tablet interacts with carbamazepine, which is used to prevent and control seizures. When carbamazepine is used with Ultracet, the pain-reducing effect of Ultracet is reduced, and the breakdown or elimination of Ultracet is increased. Ultracet should not be used in combination with carbamazepine.
There may be an interaction of Ultracet with triptans, which are used to treat migraine. Patients taking triptans in combination with Ultracet may experience increased serotonergic activity in the central nervous system (serotonin syndrome). Take necessary precautions while using Ultracet in combination with triptans.
Ultracet Tablet may interact with monoamine oxidase inhibitors, which are used to treat depression. The use of Ultracet with monoamine oxidase (MAO) inhibitors may cause diarrhea, confusion, increased heartbeat, trembling, excessive sweating, seizures or coma. In patients taking MAO inhibitors, Ultracet should be given after two weeks of MAO inhibitors treatment.
Special instructions need to be followed while taking this medicine along with alcohol, which is used for sleepiness effect. Alcohol may increase sleepiness effect of Ultracet. Thus, the use of alcohol with Ultracet while using machines and driving vehicles may be dangerous. The use of alcohol or alcohol containing products should be avoided while taking Ultracet.
Your doctor’s guidelines may need to be followed while taking this medicine along with serotonergic drugs, used to treat depression. The use of Ultracet with serotonin and norepinephrine reuptake inhibitors (SNRIs), selective serotonin reuptake inhibitors (SSRIs), monoamine oxidase inhibitors (MAOIs), tricyclic antidepressants, antipsychotics may cause seizures and serotonin syndrome in the patients. The use of α2-adrenergic blockers, triptans, St. John’s Wort, lithium or linezolid may cause a life-threatening condition (called as, serotonin syndrome) in the patients. Take necessary precautions while using Ultracet in combination with serotonergic drugs.
Ultracet Tablet interacts with opioid agonists-antagonists, which are used to treat pain. When the Ultracet is used with opioid agonists-antagonists (for example, buprenorphine, nalbuphine, pentazocine), the pain-relieving effect gets reduced and increases the risk of withdrawal symptoms. Ultracet should not be used along with opioid agonists-antagonists.
Special instructions need to be followed while taking this medicine along with cytochrome 2D6 and cytochrome 3A4 inducers or inhibitors. The use of Ultracet with cytochrome 2D6 (for example, paroxetine, fluoxetine, and amitriptyline) and cytochrome 3A4 inhibitors (for example, erythromycin, ketoconazole) or inducers (for example, St. John’s Wort and rifampin) may affect the breakdown and amount of Ultracet. These patients may suffer from seizures and a life-threatening condition (called as, serotonin syndrome).
There may be an interaction of Ultracet with warfarin like compounds, which are used to prevent blood clottimg. The use of Ultracet with warfarin-like compounds may cause an increase in the blood clotting time. Regularly monitoring of the prothrombin time should be done in the patients using Ultracet together with warfarin-like compounds.
Ultracet Tablet may interact with digoxin, which is used to treat heart failure. When Ultracet is used in combination with digoxin, an increase in the level of digoxin may occur.
Ultracet Tablet may interact with other opioid derivatives (including antitussive drugs and substitutive treatments), benzodiazepines and barbiturates, which are used to treat anxiety. When the Ultracet is used with other opioid derivative drugs, barbiturates, or benzodiazepines the risk of slow and ineffective breathing increases that can result in the fatality in cases of overdose. Use this medicine with caution in such patients.
Special instructions need to be followed while taking this medicine along with other central nervous system depressants, which are used to treat anxiety and insomnia. If the Ultracet is used with other central nervous system depressants, such as other anxiolytics, sedative antidepressants, hypnotics, sedative antihistamines, centrally-acting antihypertensive drugs, neuroleptics, thalidomide and baclofen, the patient may suffer from increased central depression and the impact on alertness can cause driving and use of machines harmful. Take necessary precautions while using Ultracet in such patients.
Ultracet Tablet interacts with mirtazapine, which is used to treat depression. The use of Ultracet with mirtazapine may cause seizures and a life-threatening condition (called as, serotonin syndrome) in the patients. Use this medicine with caution in such patients.
There may be an interaction of Ultracet with seizure threshold-lowering medicines. The use of Ultracet with seizure threshold-lowering medicines (for example, tetrahydrocannabinol, mirtazapine, bupropion) may cause seizures in the patients. Take necessary precautions while using Ultracet in combination with seizure threshold-lowering medicines.
This page does not contain all the possible interactions of Ultracet Tablet. Share a list of all medicines that you use with your doctor and pharmacist. Do not start, stop, or change the dose of any medicines without the approval of your doctor.
Interactions of Ultracet by Severity
When should Ultracet be not used?
Severe allergy
This medicine is not recommended in patients who are severely allergic to tramadol, paracetamol, opioids, or any of its components. These patients may have the following symptoms if they use this medicine:
- severe itching
- hives
- tightening of airway muscles (bronchospasm)
- swelling due to fluid accumulation
- drug-induced severe allergic reaction
- severe skin reaction (Stevens-Johnson syndrome)
- swelling of the face
- swelling of the mouth
- swelling of the throat
- respiratory distress
- rash
- vomiting
Patients consuming alcohol, centrally acting analgesics, opioids, narcotics, hypnotics, or psychotropic drugs
The use of Ultracet is not recommended in these patients. This medicine may cause slow and ineffective breathing and worsens central nervous system in such patients.
Patients using monoamine oxidase inhibitors
This medicine is not recommended in patients using monoamine oxidase inhibitors (MAOIs) or who have used MAOIs in last two weeks. Patients using monoamine oxidase inhibitors may experience increased serotonergic activity in the central nervous system (serotonin syndrome). These patients may have the following symptoms if they use this medicine:
- diarrhea
- confusion
- increased heartbeat
- trembling
- excessive sweating
- coma
Abnormal functioning of the liver
The use of this medicine is not recommended in patients with abnormal functioning of the liver.
Patients with uncontrolled seizure disorders (epilepsy)
This medicine is not recommended in patients with uncontrolled seizure disorders (epilepsy).
Severe kidney disease (creatinine clearance less than 10 ml/min)
The use of this medicine is not recommended in patients with severe kidney disease (creatinine clearance less than 10 ml/min).
Severe respiratory insufficiency
This medicine is not recommended in patients with severe respiratory insufficiency.
Traveling With Medication
- Ensure that you carry enough doses of each of your prescription medicines to last the entire trip. The best place to store your medicines is in the carry on baggage. However, while flying, if carrying liquid medicines, make sure you do not go over the limits imposed for carry-on liquids.
- While traveling overseas, make sure that you can carry each of your prescription medicines legally to your destination country. One way to ensure this is by checking with your destination country’s embassy or website.
- Make sure that you carry each of your medicines in their original packaging, which should typically include your name and address, and the details of the prescribing doctor.
- If your travel involves crossing time zones, and you are required to take your medicine as per a fixed schedule, make sure that you adjust for the change in time.
Expired Medication
Taking a single dose of expired Ultracet is unlikely to cause a side-effect. However, please discuss with your doctor or pharmacist, if you feel unwell or sick. An expired medicine may become ineffective in treating your prescribed conditions. To be on the safe side, it is important not to use an expired drug. You are much safer by always keeping a fresh supply of unexpired medicines.
Safe Disposal of Medication
- If there are disposal instructions on the package, please follow the instructions.
- If there are medicine take-back programs in your country, you should contact the respective authority to arrange for the disposal of the medicine. For example, in the USA, the Drug Enforcement Administration regularly hosts National Prescription Drug Take-Back events.
- If there are no take-back programs, mix the medicine with dirt and place them in a sealed plastic bag. Throw the plastic bag in your household trash. Separately, remove all personal information including the prescription label from the medicine packaging and then dispose off the container.
- If specifically indicated on the medicine package that it needs to be flushed down the toilet when no longer needed, perform the required step.
This page provides information for Ultracet Tablet .
-
Pain
Pain is a feeling triggered in the nervous system. Pain may be …
-
Headache
Almost everyone has had a headache. Headache is the most common …
-
Period Pain
Menstruation, or period, is normal vaginal bleeding that happens …
-
Back Pain
If you’ve ever groaned, «Oh, my aching back!», you are not …
Lake Erie Medical & Surgical Supply DBA Quality Care Products LLC
ULTRACET (TRAMADOL HYDROCHLORIDE/ACETAMINOPHEN) TABLETS
FULL PRESCRIBING INFORMATION: CONTENTS*
- Full Prescribing Information
- ULTRACET DESCRIPTION
- CLINICAL PHARMACOLOGY
- Pharmacodynamics
- Pharmacokinetics
- Special Populations
- CLINICAL STUDIES
- Single Dose Studies for Treatment of Acute Pain
- ULTRACET INDICATIONS AND USAGE
- ULTRACET CONTRAINDICATIONS
- WARNINGS
- Seizure Risk
- Serotonin Syndrome Risk
- Anaphylactoid Reactions
- Respiratory Depression
- Interaction With Central Nervous System (CNS) Depressants
- Increased Intracranial Pressure or Head Trauma
- Use in Ambulatory Patients
- Use With MAO Inhibitors and Serotonin Re-uptake Inhibitors
- Use With Alcohol
- Use With Other Acetaminophen-containing Products
- Withdrawal
- Physical Dependence and Abuse
- Risk of Overdosage
- PRECAUTIONS
- General
- Pediatric Use
- Geriatric Use
- Acute Abdominal Conditions
- Use in Renal Disease
- Use in Hepatic Disease
- Information for Patients
- Drug Interactions
- Carcinogenesis, Mutagenesis, Impairment of Fertility
- Pregnancy
- Labor and Delivery
- Nursing Mothers
- ULTRACET ADVERSE REACTIONS
- DRUG ABUSE AND DEPENDENCE
- OVERDOSAGE
- Tramadol
- Acetaminophen
- TREATMENT OF OVERDOSE
- ULTRACET DOSAGE AND ADMINISTRATION
- Individualization of Dose
- HOW SUPPLIED
- Image of Label
FULL PRESCRIBING INFORMATION
Full Prescribing Information
ULTRACET DESCRIPTION
ULTRACET® (tramadol hydrochloride/acetaminophen) Tablets combines two analgesics, tramadol 37.5 mg and acetaminophen 325 mg.
The chemical name for tramadol hydrochloride is (±)cis-2-[(dimethylamino)methyl]-1-(3-methoxyphenyl) cyclohexanol hydrochloride. Its structural formula is:
The molecular weight of tramadol hydrochloride is 299.84. Tramadol hydrochloride is a white, bitter, crystalline and odorless powder.
The chemical name for acetaminophen is N-acetyl-p-aminophenol. Its structural formula is:
The molecular weight of acetaminophen is 151.17. Acetaminophen is an analgesic and antipyretic agent which occurs as a white, odorless, crystalline powder, possessing a slightly bitter taste.
ULTRACET® tablets contain 37.5 mg tramadol hydrochloride and 325 mg acetaminophen and are light yellow in color. Inactive ingredients in the tablet are powdered cellulose, pregelatinized corn starch, sodium starch glycolate, corn starch, magnesium stearate, hypromellose, polyethylene glycol, polysorbate 80, titanium dioxide, iron oxide, and carnauba wax.
CLINICAL PHARMACOLOGY
The following information is based on studies of tramadol alone or acetaminophen alone, except where otherwise noted:
Pharmacodynamics
Tramadol is a centrally acting synthetic opioid analgesic. Although its mode of action is not completely understood, from animal tests, at least two complementary mechanisms appear applicable: binding of parent and M1 metabolite to µ-opioid receptors and weak inhibition of reuptake of norepinephrine and serotonin.
Opioid activity is due to both low affinity binding of the parent compound and higher affinity binding of the O-demethylated metabolite M1 to µ-opioid receptors. In animal models, M1 is up to 6 times more potent than tramadol in producing analgesia and 200 times more potent in µ-opioid binding. Tramadol-induced analgesia is only partially antagonized by the opiate antagonist naloxone in several animal tests. The relative contribution of both tramadol and M1 to human analgesia is dependent upon the plasma concentrations of each compound (see
CLINICAL PHARMACOLOGY, Pharmacokinetics
).
Tramadol has been shown to inhibit reuptake of norepinephrine and serotonin in vitro, as have some other opioid analgesics. These mechanisms may contribute independently to the overall analgesic profile of tramadol.
Apart from analgesia, tramadol administration may produce a constellation of symptoms (including dizziness, somnolence, nausea, constipation, sweating and pruritus) similar to that of other opioids.
Acetaminophen
Acetaminophen is a non-opiate, non-salicylate analgesic.
Pharmacokinetics
Tramadol is administered as a racemate and both the [-] and [+] forms of both tramadol and M1 are detected in the circulation. The pharmacokinetics of plasma tramadol and acetaminophen following oral administration of one ULTRACET® tablet are shown in Table 1. Tramadol has a slower absorption and longer half-life when compared to acetaminophen.
Parameter For acetaminophen, Cmax was measured asµg/mL. For acetaminophen, Cmax was measured asµg/mL.
|
(+)-Tramadol | (-)-Tramadol | (+)-M1 | (-)-M1 | acetaminophen | |||||
| Cmax (ng/mL) | 64.3 | (9.3) | 55.5 | (8.1) | 10.9 | (5.7) | 12.8 | (4.2) | 4.2 | (0.8) |
| tmax (h) | 1.8 | (0.6) | 1.8 | (0.7) | 2.1 | (0.7) | 2.2 | (0.7) | 0.9 | (0.7) |
| CL/F (mL/min) | 588 | (226) | 736 | (244) | — | — | — | — | 365 | (84) |
| t1/2 (h) | 5.1 | (1.4) | 4.7 | (1.2) | 7.8 | (3.0) | 6.2 | (1.6) | 2.5 | (0.6) |
A single dose pharmacokinetic study of ULTRACET® in volunteers showed no drug interactions between tramadol and acetaminophen. Upon multiple oral dosing to steady state, however, the bioavailability of tramadol and metabolite M1 was lower for the combination tablets compared to tramadol administered alone. The decrease in AUC was 14% for (+)-tramadol, 10.4% for (-)-tramadol, 11.9% for (+)-M1 and 24.2% for (-)-M1. The cause of this reduced bioavailability is not clear. Following single or multiple dose administration of ULTRACET®, no significant change in acetaminophen pharmacokinetics was observed when compared to acetaminophen given alone.
Absorption
The absolute bioavailability of tramadol from ULTRACET® tablets has not been determined. Tramadol hydrochloride has a mean absolute bioavailability of approximately 75% following administration of a single 100 mg oral dose of ULTRAM® tablets. The mean peak plasma concentration of racemic tramadol and M1 after administration of two ULTRACET® tablets occurs at approximately two and three hours, respectively, post-dose.
Peak plasma concentrations of acetaminophen occur within one hour and are not affected by co-administration with tramadol. Oral absorption of acetaminophen following administration of ULTRACET® occurs primarily in the small intestine.
Food Effects
When ULTRACET® was administered with food, the time to peak plasma concentration was delayed for approximately 35 minutes for tramadol and almost one hour for acetaminophen. However, peak plasma concentration or the extent of absorption of either tramadol or acetaminophen were not affected. The clinical significance of this difference is unknown.
Distribution
The volume of distribution of tramadol was 2.6 and 2.9 L/kg in male and female subjects, respectively, following a 100 mg intravenous dose. The binding of tramadol to human plasma proteins is approximately 20% and binding also appears to be independent of concentration up to 10 µg/mL. Saturation of plasma protein binding occurs only at concentrations outside the clinically relevant range.
Acetaminophen appears to be widely distributed throughout most body tissues except fat. Its apparent volume of distribution is about 0.9 L/kg. A relative small portion (~20%) of acetaminophen is bound to plasma protein.
Metabolism
Following oral administration, tramadol is extensively metabolized by a number of pathways, including CYP2D6 and CYP3A4, as well as by conjugation of parent and metabolites. Approximately 30% of the dose is excreted in the urine as unchanged drug, whereas 60% of the dose is excreted as metabolites. The major metabolic pathways appear to be N — and O— demethylation and glucuronidation or sulfation in the liver. Metabolite M1 (O -desmethyltramadol) is pharmacologically active in animal models. Formation of M1 is dependent on CYP2D6 and as such is subject to inhibition, which may affect the therapeutic response (see
PRECAUTIONS, Drug Interactions
).
Approximately 7% of the population has reduced activity of the CYP2D6 isoenzyme of cytochrome P450. These individuals are «poor metabolizers» of debrisoquine, dextromethorphan, tricyclic antidepressants, among other drugs. Based on a population PK analysis of Phase 1 studies in healthy subjects, concentrations of tramadol were approximately 20% higher in «poor metabolizers» versus «extensive metabolizers», while M1 concentrations were 40% lower. In vitro drug interaction studies in human liver microsomes indicates that inhibitors of CYP2D6 such as fluoxetine and its metabolite norfluoxetine, amitriptyline and quinidine inhibit the metabolism of tramadol to various degrees. The full pharmacological impact of these alterations in terms of either efficacy or safety is unknown. Concomitant use of SEROTONIN re-uptake INHIBITORS and MAO INHIBITORS may enhance the risk of adverse events, including seizure (see
WARNINGS
) and serotonin syndrome.
Acetaminophen is primarily metabolized in the liver by first-order kinetics and involves three principal separate pathways:
- a)conjugation with glucuronide;
- b)conjugation with sulfate; and
- c)oxidation via the cytochrome, P450-dependent, mixed-function oxidase enzyme pathway to form a reactive intermediate metabolite, which conjugates with glutathione and is then further metabolized to form cysteine and mercapturic acid conjugates. The principal cytochrome P450 isoenzyme involved appears to be CYP2E1, with CYP1A2 and CYP3A4 as additional pathways.
In adults, the majority of acetaminophen is conjugated with glucuronic acid and, to a lesser extent, with sulfate. These glucuronide-, sulfate-, and glutathione-derived metabolites lack biologic activity. In premature infants, newborns, and young infants, the sulfate conjugate predominates.
Elimination
Tramadol is eliminated primarily through metabolism by the liver and the metabolites are eliminated primarily by the kidneys. The plasma elimination half-lives of racemic tramadol and M1 are approximately 5–6 and 7 hours, respectively, after administration of ULTRACET®. The apparent plasma elimination half-life of racemic tramadol increased to 7–9 hours upon multiple dosing of ULTRACET®.
The half-life of acetaminophen is about 2 to 3 hours in adults. It is somewhat shorter in children and somewhat longer in neonates and in cirrhotic patients. Acetaminophen is eliminated from the body primarily by formation of glucuronide and sulfate conjugates in a dose-dependent manner. Less than 9% of acetaminophen is excreted unchanged in the urine.
Special Populations
Renal
The pharmacokinetics of ULTRACET® in patients with renal impairment has not been studied. Based on studies using tramadol alone, excretion of tramadol and metabolite M1 is reduced in patients with creatinine clearance of less than 30 mL/min, adjustment of dosing regimen in this patient population is recommended (see
DOSAGE AND ADMINISTRATION
). The total amount of tramadol and M1 removed during a 4-hour dialysis period is less than 7% of the administered dose based on studies using tramadol alone.
Hepatic
The pharmacokinetics and tolerability of ULTRACET® in patients with impaired hepatic function has not been studied. Since tramadol and acetaminophen are both extensively metabolized by the liver, the use of ULTRACET® in patients with hepatic impairment is not recommended (see
PRECAUTIONS
and
DOSAGE AND ADMINISTRATION
).
Geriatric
A population pharmacokinetic analysis of data obtained from a clinical trial in patients with chronic pain treated with ULTRACET® which included 55 patients between 65 and 75 years of age and 19 patients over 75 years of age, showed no significant changes in pharmacokinetics of tramadol and acetaminophen in elderly patients with normal renal and hepatic function (see
PRECAUTIONS, Geriatric Use
).
Gender
Tramadol clearance was 20% higher in female subjects compared to males on four phase I studies of ULTRACET® in 50 male and 34 female healthy subjects. The clinical significance of this difference is unknown.
Pediatric
Pharmacokinetics of ULTRACET® tablets has not been studied in pediatric patients below 16 years of age.
CLINICAL STUDIES
Single Dose Studies for Treatment of Acute Pain
In pivotal single-dose studies in acute pain, two tablets of ULTRACET® administered to patients with pain following oral surgical procedures provided greater relief than placebo or either of the individual components given at the same dose. The onset of pain relief after ULTRACET® was faster than tramadol alone. Onset of analgesia occurred in less than one hour. The duration of pain relief after ULTRACET® was longer than acetaminophen alone. Analgesia was generally comparable to that of the comparator, ibuprofen.
ULTRACET INDICATIONS AND USAGE
ULTRACET® is indicated for the short-term (five days or less) management of acute pain.
ULTRACET CONTRAINDICATIONS
ULTRACET® should not be administered to patients who have previously demonstrated hypersensitivity to tramadol, acetaminophen, any other component of this product or opioids. ULTRACET® is contraindicated in any situation where opioids are contraindicated, including acute intoxication with any of the following: alcohol, hypnotics, narcotics, centrally acting analgesics, opioids or psychotropic drugs. ULTRACET® may worsen central nervous system and respiratory depression in these patients.
WARNINGS
Seizure Risk
Seizures have been reported in patients receiving tramadol within the recommended dosage range. Spontaneous post-marketing reports indicate that seizure risk is increased with doses of tramadol above the recommended range. Concomitant use of tramadol increases the seizure risk in patients taking:
- Selective serotonin reuptake inhibitors (SSRI antidepressants or anorectics),
- Tricyclic antidepressants (TCAs), and other tricyclic compounds (e.g., cyclobenzaprine, promethazine, etc.), or
- Other opioids.
Administration of tramadol may enhance the seizure risk in patients taking:
- MAO inhibitors (see also
WARNINGS, Use with MAO Inhibitors and Serotonin Re-uptake Inhibitors
), - Neuroleptics, or
- Other drugs that reduce the seizure threshold.
Risk of convulsions may also increase in patients with epilepsy, those with a history of seizures, or in patients with a recognized risk for seizure (such as head trauma, metabolic disorders, alcohol and drug withdrawal, CNS infections). In tramadol overdose, naloxone administration may increase the risk of seizure.
Serotonin Syndrome Risk
The development of a potentially life-threatening serotonin syndrome may occur with the use of tramadol products, including ULTRACET®, particularly with concomitant use of serotonergic drugs such as SSRIs, SNRIs, TCAs, MAOIs, and triptans, with drugs which impair metabolism of serotonin (including MAOIs), and with drugs which impair metabolism of tramadol (CYP2D6 and CYP3A4 inhibitors). This may occur within the recommended dose (see CLINICAL PHARMACOLOGY, Pharmacokinetics).
Serotonin syndrome may include mental-status changes (e.g., agitation, hallucinations, coma), autonomic instability (e.g., tachycardia, labile blood pressure, hyperthermia), neuromuscular aberrations (e.g., hyperreflexia, incoordination) and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea).
Anaphylactoid Reactions
Serious and rarely fatal anaphylactoid reactions have been reported in patients receiving therapy with tramadol. When these events do occur it is often following the first dose. Other reported allergic reactions include pruritus, hives, bronchospasm, angioedema, toxic epidermal necrolysis and Stevens-Johnson syndrome. Patients with a history of anaphylactoid reactions to codeine and other opioids may be at increased risk and therefore should not receive ULTRACET® (see
CONTRAINDICATIONS
).
Respiratory Depression
Administer ULTRACET® cautiously in patients at risk for respiratory depression. In these patients, alternative non-opioid analgesics should be considered. When large doses of tramadol are administered with anesthetic medications or alcohol, respiratory depression may result. Respiratory depression should be treated as an overdose. If naloxone is to be administered, use cautiously because it may precipitate seizures (see
WARNINGS, Seizure Risk
and
OVERDOSAGE
).
Interaction With Central Nervous System (CNS) Depressants
ULTRACET® should be used with caution and in reduced dosages when administered to patients receiving CNS depressants such as alcohol, opioids, anesthetic agents, narcotics, phenothiazines, tranquilizers or sedative hypnotics. Tramadol increases the risk of CNS and respiratory depression in these patients.
Increased Intracranial Pressure or Head Trauma
ULTRACET® should be used with caution in patients with increased intracranial pressure or head injury. The respiratory depressant effects of opioids include carbon dioxide retention and secondary elevation of cerebrospinal fluid pressure and may be markedly exaggerated in these patients. Additionally, pupillary changes (miosis) from tramadol may obscure the existence, extent, or course of intracranial pathology. Clinicians should also maintain a high index of suspicion for adverse drug reaction when evaluating altered mental status in these patients if they are receiving ULTRACET (see
WARNINGS, Respiratory Depression
).
Use in Ambulatory Patients
Tramadol may impair the mental and or physical abilities required for the performance of potentially hazardous tasks such as driving a car or operating machinery. The patient using this drug should be cautioned accordingly.
Use With MAO Inhibitors and Serotonin Re-uptake Inhibitors
Use ULTRACET® with great caution in patients taking monoamine oxidase inhibitors. Animal studies have shown increased deaths with combined administration of MAO inhibitors and tramadol. Concomitant use of tramadol with MAO inhibitors or SSRI’s increases the risk of adverse events, including seizure and serotonin syndrome.
Use With Alcohol
ULTRACET® should not be used concomitantly with alcohol consumption. The use of ULTRACET® in patients with liver disease is not recommended.
Use With Other Acetaminophen-containing Products
Due to the potential for acetaminophen hepatotoxicity at doses higher than the recommended dose, ULTRACET® should not be used concomitantly with other acetaminophen-containing products.
Withdrawal
Withdrawal symptoms may occur if ULTRACET® is discontinued abruptly (see
DRUG ABUSE AND DEPENDENCE
). These symptoms may include: anxiety, sweating, insomnia, rigors, pain, nausea, tremors, diarrhea, upper respiratory symptoms, piloerection, and rarely hallucinations. Other symptoms that have been seen less frequently with ULTRACET® discontinuation include: panic attacks, severe anxiety, and paresthesias. Clinical experience suggests that withdrawal symptoms may be avoided by tapering ULTRACET® at the time of discontinuation.
Physical Dependence and Abuse
Tramadol may induce psychic and physical dependence of the morphine-type (µ-opioid) (see
DRUG ABUSE AND DEPENDENCE
). Tramadol should not be used in opioid-dependent patients. Tramadol has been shown to reinitiate physical dependence in some patients that have been previously dependent on other opioids. Dependence and abuse, including drug-seeking behavior and taking illicit actions to obtain the drug are not limited to those patients with prior history of opioid dependence.
Risk of Overdosage
Serious potential consequences of overdosage with tramadol are central nervous system depression, respiratory depression and death. In treating an overdose, primary attention should be given to maintaining adequate ventilation along with general supportive treatment (see
OVERDOSAGE
).
Serious potential consequences of overdosage with acetaminophen are hepatic (centrilobular) necrosis, leading to hepatic failure and death. Emergency help should be sought immediately and treatment initiated immediately if overdose is suspected, even if symptoms are not apparent.
PRECAUTIONS
General
The recommended dose of ULTRACET® should not be exceeded.
Do not co-administer ULTRACET® with other tramadol or acetaminophen-containing products (see
WARNINGS, Use With Other Acetaminophen-containing Products
and
Risk of Overdosage
).
Pediatric Use
The safety and effectiveness of ULTRACET® has not been studied in the pediatric population.
Geriatric Use
In general, dose selection for an elderly patient should be cautious, reflecting the greater frequency of decreased hepatic, renal, or cardiac function; of concomitant disease and multiple drug therapy.
Acute Abdominal Conditions
The administration of ULTRACET® may complicate the clinical assessment of patients with acute abdominal conditions.
Use in Renal Disease
ULTRACET® has not been studied in patients with impaired renal function. Experience with tramadol suggests that impaired renal function results in a decreased rate and extent of excretion of tramadol and its active metabolite, M1. In patients with creatinine clearances of less than 30 mL/min, it is recommended that the dosing interval of ULTRACET® be increased not to exceed 2 tablets every 12 hours.
Use in Hepatic Disease
ULTRACET® has not been studied in patients with impaired hepatic function. The use of ULTRACET® in patients with hepatic impairment is not recommended (see
WARNINGS, Use With Alcohol
).
Information for Patients
- Patients should be informed that ULTRACET® may cause seizures and/or serotonin syndrome with concomitant use of serotonergic agents (including SSRIs, SNRIs, and triptans) or drugs that significantly reduce the metabolic clearance of tramadol.
- ULTRACET® may impair mental or physical abilities required for the performance of potentially hazardous tasks such as driving a car or operating machinery.
- ULTRACET® should not be taken with alcohol containing beverages.
- The patient should be instructed not to take ULTRACET® in combination with other tramadol or acetaminophen-containing products, including over-the-counter preparations.
- ULTRACET® should be used with caution when taking medications such as tranquilizers, hypnotics or other opiate containing analgesics.
- The patient should be instructed to inform the physician if they are pregnant, think they might become pregnant, or are trying to become pregnant (see
PRECAUTIONS, Labor and Delivery
). - The patient should understand the single-dose and 24-hour dose limit and the time interval between doses, since exceeding these recommendations can result in respiratory depression, seizures, hepatic toxicity and death.
Drug Interactions
CYP2D6 and CYP3A4 Inhibitors
Concomitant administration of CYP2D6 and/or CYP3A4 inhibitors (see
CLINICAL PHARMACOLOGY, Pharmacokinetics
), such as quinidine, fluoxetine, paroxetine and amitriptyline (CYP2D6 inhibitors), and ketoconazole and erythromycin (CYP3A4 inhibitors), may reduce metabolic clearance of tramadol increasing the risk for serious adverse events including seizures and serotonin syndrome.
Serotonergic Drugs
There have been postmarketing reports of serotonin syndrome with use of tramadol and SSRIs/SNRIs or MAOIs and α2-adrenergic blockers. Caution is advised when ULTRACET® is coadministered with other drugs that may affect the serotonergic neurotransmitter systems, such as SSRIs, MAOIs, triptans, linezolid (an antibiotic which is a reversible non-selective MAOI), lithium, or St. John’s Wort. If concomitant treatment of ULTRACET® with a drug affecting the serotonergic neurotransmitter system is clinically warranted, careful observation of the patient is advised, particularly during treatment initiation and dose increases (see
WARNINGS, Serotonin Syndrome
).
Triptans
Based on the mechanism of action of tramadol and the potential for serotonin syndrome, caution is advised when ULTRACET® is coadministered with a triptan. If concomitant treatment of ULTRACET® with a triptan is clinically warranted, careful observation of the patient is advised, particularly during treatment initiation and dose increases (see
WARNINGS, Serotonin Syndrome
).
Use With Carbamazepine
Patients taking carbamazepine may have a significantly reduced analgesic effect of tramadol. Because carbamazepine increases tramadol metabolism and because of the seizure risk associated with tramadol, concomitant administration of ULTRACET® and carbamazepine is not recommended.
Use With Quinidine
Tramadol is metabolized to M1 by CYP2D6. Quinidine is a selective inhibitor of that isoenzyme; so that concomitant administration of quinidine and tramadol results in increased concentrations of tramadol and reduced concentrations of M1. The clinical consequences of these findings are unknown. In vitro drug interaction studies in human liver microsomes indicate that tramadol has no effect on quinidine metabolism.
Potential for Other Drugs to Affect Tramadol
In vitro drug interaction studies in human liver microsomes indicate that concomitant administration with inhibitors of CYP2D6 such as fluoxetine, paroxetine, and amitriptyline could result in some inhibition of the metabolism of tramadol.
Potential for Tramadol to Affect Other Drugs
In vitro studies indicate that tramadol is unlikely to inhibit the CYP3A4-mediated metabolism of other drugs when tramadol is administered concomitantly at therapeutic doses. Tramadol does not appear to induce its own metabolism in humans, since observed maximal plasma concentrations after multiple oral doses are higher than expected based on single-dose data. Tramadol is a mild inducer of selected drug metabolism pathways measured in animals.
Use With Cimetidine
Concomitant administration of ULTRACET® and cimetidine has not been studied. Concomitant administration of tramadol and cimetidine does not result in clinically significant changes in tramadol pharmacokinetics. Therefore, no alteration of the ULTRACET® dosage regimen is recommended.
Use With Digoxin
Post-marketing surveillance of tramadol has revealed rare reports of digoxin toxicity.
Use With Warfarin Like Compounds
Post-marketing surveillance of both tramadol and acetaminophen individual products have revealed rare alterations of warfarin effect, including elevation of prothrombin times.
While such changes have been generally of limited clinical significance for the individual products, periodic evaluation of prothrombin time should be performed when ULTRACET® and warfarin-like compounds are administered concurrently.
Carcinogenesis, Mutagenesis, Impairment of Fertility
There are no animal or laboratory studies on the combination product (tramadol and acetaminophen) to evaluate carcinogenesis, mutagenesis, or impairment of fertility.
A slight but statistically significant increase in two common murine tumors, pulmonary and hepatic, was observed in a mouse carcinogenicity study, particularly in aged mice. Mice were dosed orally up to 30 mg/kg (90 mg/m2 or 0.5 times the maximum daily human tramadol dosage of 185 mg/m2) for approximately two years, although the study was not done with the Maximum Tolerated Dose. This finding is not believed to suggest risk in humans. No such finding occurred in rat carcinogenicity study (dosing orally up to 30 mg/kg, 180 mg/m2, or 1 time the maximum daily human tramadol dosage).
Tramadol was not mutagenic in the following assays: Ames Salmonella microsomal activation test, CHO/HPRT mammalian cell assay, mouse lymphoma assay (in the absence of metabolic activation), dominant lethal mutation tests in mice, chromosome aberration test in Chinese hamsters, and bone marrow micronucleus tests in mice and Chinese hamsters. Weakly mutagenic results occurred in the presence of metabolic activation in the mouse lymphoma assay and micronucleus test in rats. Overall, the weight of evidence from these tests indicates that tramadol does not pose a genotoxic risk to humans.
No effects on fertility were observed for tramadol at oral dose levels up to 50 mg/kg (350 mg/m2) in male rats and 75 mg/kg (450 mg/m2) in female rats. These dosages are 1.6 and 2.4 times the maximum daily human tramadol dosage of 185 mg/m2.
Pregnancy
Teratogenic Effects: Pregnancy Category C
No drug-related teratogenic effects were observed in the progeny of rats treated orally with tramadol and acetaminophen. The tramadol/acetaminophen combination product was shown to be embryotoxic and fetotoxic in rats at a maternally toxic dose, 50/434 mg/kg tramadol/acetaminophen (300/2604 mg/m2 or 1.6 times the maximum daily human tramadol/acetaminophen dosage of 185/1591 mg/m2), but was not teratogenic at this dose level. Embryo and fetal toxicity consisted of decreased fetal weights and increased supernumerary ribs.
Non-teratogenic Effects:
Tramadol alone was evaluated in peri- and post-natal studies in rats. Progeny of dams receiving oral (gavage) dose levels of 50 mg/kg (300 mg/m2 or 1.6 times the maximum daily human tramadol dosage) or greater had decreased weights, and pup survival was decreased early in lactation at 80 mg/kg (480 mg/m2 or 2.6 times the maximum daily human tramadol dosage).
There are no adequate and well-controlled studies in pregnant women. ULTRACET® should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. Neonatal seizures, neonatal withdrawal syndrome, fetal death and still birth have been reported with tramadol hydrochloride during post-marketing.
Labor and Delivery
ULTRACET® should not be used in pregnant women prior to or during labor unless the potential benefits outweigh the risks. Safe use in pregnancy has not been established. Chronic use during pregnancy may lead to physical dependence and post-partum withdrawal symptoms in the newborn (see
DRUG ABUSE AND DEPENDENCE
). Tramadol has been shown to cross the placenta. The mean ratio of serum tramadol in the umbilical veins compared to maternal veins was 0.83 for 40 women given tramadol during labor.
The effect of ULTRACET®, if any, on the later growth, development, and functional maturation of the child is unknown.
Nursing Mothers
ULTRACET® is not recommended for obstetrical preoperative medication or for post-delivery analgesia in nursing mothers because its safety in infants and newborns has not been studied.
Following a single IV 100 mg dose of tramadol, the cumulative excretion in breast milk within 16 hours post-dose was 100 µg of tramadol (0.1% of the maternal dose) and 27 µg of M1.
ULTRACET ADVERSE REACTIONS
Table 2 reports the incidence rate of treatment-emergent adverse events over five days of ULTRACET® use in clinical trials (subjects took an average of at least 6 tablets per day).
| Body System | ULTRACET (N=142) |
| Preferred Term | (%) |
| Gastrointestinal System Disorders | |
| Constipation | 6 |
| Diarrhea | 3 |
| Nausea | 3 |
| Dry Mouth | 2 |
| Psychiatric Disorders | |
| Somnolence | 6 |
| Anorexia | 3 |
| Insomnia | 2 |
| Central & Peripheral Nervous System | |
| Dizziness | 3 |
| Skin and Appendages | |
| Sweating Increased | 4 |
| Pruritus | 2 |
Reproductive Disorders, Male  Number of males = 62 Number of males = 62 |
|
| Prostatic Disorder | 2 |
Incidence at least 1%, causal relationship at least possible or greater: the following lists adverse reactions that occurred with an incidence of at least 1% in single-dose or repeated-dose clinical trials of ULTRACET®.
Body as a Whole – Asthenia, fatigue, hot flushes
Central and Peripheral Nervous System – Dizziness, headache, tremor
Gastrointestinal System – Abdominal pain, constipation, diarrhea, dyspepsia, flatulence, dry mouth, nausea, vomiting
Psychiatric Disorders – Anorexia, anxiety, confusion, euphoria, insomnia, nervousness, somnolence
Skin and Appendages – Pruritus, rash, increased sweating.
Selected Adverse events occurring at less than 1%: the following lists clinically relevant adverse reactions that occurred with an incidence of less than 1% in ULTRACET® clinical trials.
Body as a Whole – Chest pain, rigors, syncope, withdrawal syndrome
Cardiovascular Disorders– Hypertension, aggravated hypertension, hypotension
Central and Peripheral Nervous System – Ataxia, convulsions, hypertonia, migraine, aggravated migraine, involuntary muscle contractions, paresthesias, stupor, vertigo
Gastrointestinal System– Dysphagia, melena, tongue edema
Hearing and Vestibular Disorders – Tinnitus
Heart Rate and Rhythm Disorders – Arrhythmia, palpitation, tachycardia
Liver and Biliary System– Hepatic function abnormal
Metabolic and Nutritional Disorders – Weight decrease
Psychiatric Disorders – Amnesia, depersonalization, depression, drug abuse, emotional lability, hallucination, impotence, paroniria, abnormal thinking
Red Blood Cell Disorders – Anemia
Respiratory System – Dyspnea
Urinary System – Albuminuria, micturition disorder, oliguria, urinary retention
Vision Disorders – Abnormal vision
Other clinically significant adverse experiences previously reported with tramadol hydrochloride.
Other events which have been reported with the use of tramadol products and for which a causal association has not been determined include: vasodilation, orthostatic hypotension, myocardial ischemia, pulmonary edema, allergic reactions (including anaphylaxis and urticaria, Stevens-Johnson syndrome/TENS), cognitive dysfunction, difficulty concentrating, depression, suicidal tendency, hepatitis liver failure and gastrointestinal bleeding. Reported laboratory abnormalities included elevated creatinine and liver function tests. Serotonin syndrome (whose symptoms may include mental status change, hyperreflexia, fever, shivering, tremor, agitation, diaphoresis, seizures and coma) has been reported with tramadol when used concomitantly with other serotonergic agents such as SSRIs and MAOIs.
Other clinically significant adverse experiences previously reported with acetaminophen.
Allergic reactions (primarily skin rash) or reports of hypersensitivity secondary to acetaminophen are rare and generally controlled by discontinuation of the drug and, when necessary, symptomatic treatment.
DRUG ABUSE AND DEPENDENCE
Tramadol may induce psychic and physical dependence of the morphine-type (µ-opioid) (see
WARNINGS
). Dependence and abuse, including drug-seeking behavior and taking illicit actions to obtain the drug are not limited to those patients with a prior history of opioid dependence. The risk in patients with substance abuse has been observed to be higher. Tramadol is associated with craving and tolerance development. Withdrawal symptoms may occur if tramadol is discontinued abruptly. These symptoms may include: anxiety, sweating, insomnia, rigors, pain, nausea, tremors, diarrhea, upper respiratory symptoms, piloerection and rarely hallucinations. Other symptoms that have been seen less frequently with ULTRACET® discontinuation include: panic attacks, severe anxiety, and paresthesias. Clinical experience suggests that withdrawal symptoms may be relieved by reinstitution of opioid therapy followed by a gradual, tapered dose reduction of the medication combined with symptomatic support.
OVERDOSAGE
ULTRACET® is a combination product. The clinical presentation of overdose may include the signs and symptoms of tramadol toxicity, acetaminophen toxicity or both. The initial symptoms of tramadol overdosage may include respiratory depression and or seizures. The initial symptoms seen within the first 24 hours following an acetaminophen overdose are: anorexia, nausea, vomiting, malaise, pallor and diaphoresis.
Tramadol
Serious potential consequences of overdosage are respiratory depression, lethargy, coma, seizure, cardiac arrest and death (see
WARNINGS
). Fatalities have been reported in post marketing in association with both intentional and unintentional overdose with tramadol.
Acetaminophen
Serious potential consequences of overdosage with acetaminophen are hepatic centrilobular necrosis, leading to hepatic failure and death. Renal tubular necrosis, hypoglycemia and coagulation defects also may occur. Early symptoms following a potentially hepatotoxic overdose may include: nausea, vomiting, diaphoresis and general malaise. Clinical and laboratory evidence of hepatic toxicity may not be apparent until 48 to 72 hours post ingestion.
TREATMENT OF OVERDOSE
A single or multiple overdose with ULTRACET® may be a potentially lethal polydrug overdose, and consultation with a regional poison control center is recommended.
In treating an overdose of ULTRACET®, primary attention should be given to maintaining adequate ventilation along with general supportive treatment. While naloxone will reverse some, but not all, symptoms caused by overdosage with tramadol, the risk of seizures is also increased with naloxone administration. In animals, convulsions following the administration of toxic doses of tramadol could be suppressed with barbiturates or benzodiazepines but were increased with naloxone. Naloxone administration did not change the lethality of an overdose in mice. Based on experience with tramadol, hemodialysis is not expected to be helpful in an overdose because it removes less than 7% of the administered dose in a 4-hour dialysis period.
Standard recommendations should be followed for the treatment of acetaminophen overdose.
ULTRACET DOSAGE AND ADMINISTRATION
For the short-term (five days or less) management of acute pain, the recommended dose of ULTRACET® is 2 tablets every 4 to 6 hours as needed for pain relief up to a maximum of 8 tablets per day.
Individualization of Dose
In patients with creatinine clearances of less than 30 mL/min, it is recommended that the dosing interval of ULTRACET® be increased not to exceed 2 tablets every 12 hours. Dose selection for an elderly patient should be cautious, in view of the potential for greater sensitivity to adverse events.
HOW SUPPLIED
ULTRACET® (tramadol hydrochloride/acetaminophen) Tablets with tramadol 37.5 mg and acetaminophen 325 mg are light yellow, coated, capsule-shaped tablets imprinted «O-M» on one side and «650» on the other are available as follows:
| 120’s: | NDC 21695-143-72 | Bottles of 120 tablets |
Dispense in a tight container. Store at 25°C (77°F); excursions permitted to 15 – 30°C (59 – 86°F).
Manufactured by:
Janssen Ortho, LLC
Gurabo, Puerto Rico 00778
Distributed by:
OMP DIVISION
ORTHO-McNEIL PHARMACEUTICAL, INC.
Raritan, New Jersey 08869
Image of Label

ULTRACET
tramadol hydrochloride and acetaminophen TABLET
Product Information |
|||
|---|---|---|---|
| Product Type | Human prescription drug label | Item Code (Source) | NDC:49999-118(NDC:0045-0650) |
| Route of Administration | ORAL | DEA Schedule |
Active Ingredient/Active Moiety |
||
|---|---|---|
| Ingredient Name | Basis of Strength | Strength |
| TRAMADOL HYDROCHLORIDE TRAMADOL | 37.5 mg | |
| ACETAMINOPHEN ACETAMINOPHEN | 325 mg |
Inactive Ingredients |
|
|---|---|
| Ingredient Name | Strength |
| POWDERED CELLULOSE | |
| STARCH, CORN | |
| SODIUM STARCH GLYCOLATE TYPE A POTATO | |
| MAGNESIUM STEARATE | |
| HYPROMELLOSES | |
| polyethylene glycol | |
| polysorbate 80 | |
| titanium dioxide | |
| ferric oxide red | |
| carnauba wax |
Product Characteristics |
|||
|---|---|---|---|
| Color | Size | Imprint Code | Shape |
| YELLOW (light yellow) | 15 mm | O;M;650 | OVAL |
Packaging |
||||
|---|---|---|---|---|
| # | Item Code | Package Description | Marketing Start Date | Marketing End Date |
| 1 | NDC:49999-118-30 | 30 in 1 BOTTLE |
Marketing Information |
|||
|---|---|---|---|
| Marketing Category | Application Number or Monograph Citation | Marketing Start Date | Marketing End Date |
| NDA | NDA021123 | 2012-03-20 |
1. Is Ultracet A Narcotic?
Yes. Tramadol present within Ultracet is a specific narcotic belonging to the class of opioids. It acts on the central nervous system to reduce moderate to acute pain in patients. Tramadol reduces pain and amplifies one’s feeling of pleasure and hence is highly addictive.
2. Is Ultracet An Opioid?
Yes. Ultracet contains Tramadol as an opioid, a Schedule IV class of drugs; opioids relieve acute pain. They surpass the blood-brain barrier and bind to receptors present in the brain to alleviate pain and uplift happiness. In moderate doses, it is beneficial.
3. What Does Ultracet Look Like?
Ultracet tablets available on the market look like elliptical-shaped tablets, white or pale white, with strengths imprinted on the tablet. Depending on the various strengths, sizes, different brands, and marketing companies, the appearances may vary.
The most available strength is 325 mg/37.5 mg combination of Tramadol hydrochloride and Acetaminophen.
4. Is Ultracet A Steroid?
No. Ultracet is a combination of Acetaminophen and Tramadol, manufactured artificially to cause pain relief. Steroids are an adjuvant to opioids medication to reduce pain and also help improve other beneficial symptoms like asthma, inflammation, arthritis. etc. Whereas, Ultracet is a non-steroidal, narcotic-based analgesic that is used primarily for pain management.
5. Is Ultracet An Anti Inflammatory?
No. Tramadol in it is not a steroid nor a NSAID (NonSteroidal Anti-inflammatory Drug). Hence, it doesn’t help reduce inflammation, swelling of the body, or muscle relaxation. Contrastingly, steroids typically decrease inflammation of the body by weakening the body’s immune responses and are generally taken in combination with analgesics for post-operative healing.
6. Is Ultracet Harmful?
Yes. Ultracet contains an opioids class of drug which is highly addictive and can cause death if misused or overdosed. Even those taking in moderation and under prescription run the risk of getting addicted and show withdrawal symptoms on cessation of Ultracet. It should be taken under strict medical guidance and kept away from children and adults equally.
7. Is Ultracet Good For Pain?
Yes. Ultracet containing Acetaminophen and Tramadol is a fast-acting pain killer and starts acting within 30 to 60 minutes after ingestion. The effects retain for 6 hours. There are also delayed-acting Ultracet tablets that take 24 to 48 hours but retain for a prolonged period.
8. Does Ultracet Affect The Kidneys?
Yes. Tramadol has not been proved to be directly nephrotoxic, but it is not advisable for kidney patients to intake Ultracet, which contains Tramadol. This is because the drug is excreted through the kidneys. Patients with kidney problems will not be able to eliminate the drug causing fatal concentrations in blood. Ultracet can also increase the blood urea and creatinine concentration, causing kidney disorders.
9. Why Is Ultracet Banned?
Ultracet is banned after the revelation of its frequent use in sportspersons, especially in competitive cycling by the World Anti-Doping Agency.
Tramadol is a synthetic opioid that causes many side effects and gradual addiction among users. The ban has been imposed considering sportspersons’ health and safety, and tests are conducted before, after, and in between competitions to prevent possible misuse.
10. Is Ultracet Still Available?
No. the genetic variation of Ultracet tablets containing Tramadol and Acetaminophen has been permanently discontinued due to adjoining side effects and the possible abuse. Tramadol is categorized as a Schedule IV controlled substance and is available under strict prescription. Moreover, the prescription can be used 5 times or 6 months only, from the date of its recommendation, after which a new prescription is required.
In case of any side effects or overdose after taking Ultracet, please consult our expert or get a medical opinion at Yashoda Hospitals-healthcare for immediate treatment.
О нас
- О нас
- Политика конфиденциальности
- Правила использования
- Обзор
- Пользы
- Побочные эффекты
- Меры предосторожности
- Взаимодействие
- Противопоказания
Обзор
Ultracet Tablet содержит следующие активные ингредиенты: Paracetamol and Tramadol. Доступен в форме tablet form.
Подробная информация, касающаяся использования, состава, дозировки, побочных эффектов Ultracet Tablet, а также отзывы пользователей предоставлены ниже:
Пользы
Побочные эффекты
Меры предосторожности
Перед началом приема данного препарата сообщите вашему врачу об уже используемых медикаментах, пищевых добавках (например, витаминах, натуральным добавкам и др.), аллергических реакциях, существующих заболеваниях и текущем состоянии здоровья (например, беременность, предстоящая операция и др.). Побочные эффекты препарата могут сильнее проявляться при определенном состоянии вашего организма. Принимайте препарат согласно указаниям вашего врача или следуйте инструкции по применению, поставляемой вместе с препаратом. Дозировка препарата зависит от вашего состояния. Сообщите вашему доктору об отсутствии изменений или ухудшении вашего состояния. Важные моменты, которые необходимо обсудить с вашим лечащим врачом, указаны ниже.
- Будьте осторожны, в случае вождения или эксплуатации тяжелой техники
- Будьте осторожны, если у вас возникли операции, в том числе стоматологической хирургии
- Возьмите за консультацией к врачу, если у вас есть травмы головы, подходит для расстройства, дыхательная проблемы, нарушение обмена веществ
- Не используйте его, если аллергия на парацетамол
- Не принимайте парацетамол, если употреблять алкогольные напитки каждый день
- Не употреблять грейпфрутовый сок
- Обратитесь к врачу, если у вас есть или были печень, почки или болезнь желудка
Если вы принимаете другие препараты или добавки, одновременно с данным препаратом, то эффективность Ultracet Tablet может измениться. Сообщите вашему лечащему врачу обо всех препаратах, витаминах и пищевых добавках, которые вы используете. Ваш врач сможет составить правильный план приема препарата, который позволит избежать негативного взаимодействия. Ultracet Tablet может вступать во взаимодействие со следующими препаратами и товарами:
- Alcohol
- Buprenorphine
- Bupropion
- Carbamazepine
- Cimetidine
- Codeine
- Interfere with certain laboratory tests
- Juxtapid mipomersen
- Ketoconazole
- Leflunomide
Повышенная чувствительность к Ultracet Tablet является противопоказанием. Кроме того, препарат Ultracet Tablet запрещено принимать при наличии у вас следующих состояний:
- Алкоголизм
- Кормление грудью
- Печеночная недостаточность
- Повышенное внутричерепное давление
- Потребление антидепрессантов
- Травмы головы
- Тяжелая почечная недостаточность
- повышенная чувствительность
Состав и активные ингредиенты
Варианты упаковки и силы препарата
Ultracet Tablet доступен в следующих упаковках со следующими вариантами интенсивности
Доступные упаковки Ultracet Tablet: 10 Tablet, 15 Tablet
Варианты интенсивности Ultracet Tablet: 50+500, 325MG+37.5MG
Часто задаваемые вопросы
-
Может ли Ultracet Tablet использоваться для боль в суставах и Интенсивная внезапная боль?
Да, боль в суставах и интенсивная внезапная боль являются самыми популярными вариантами использования Ultracet Tablet. Пожалуйста, не используйте Ultracet Tablet для боль в суставах и интенсивная внезапная боль без предварительной консультации с вашим лечащим врачом. Нажмите здесь и просмотрите результаты опроса, чтобы узнать, как именно другие пользователи применяют Ultracet Tablet.
-
Как долго я должен принимать Ultracet Tablet, прежде, чем я замечу улучшение моего состояния?
Пользователи TabletWise.com сообщили, что в тот же день и 1 неделя являются наиболее часто встречающимися сроками приема препарата до получения первых положительных эффектов. Данные показатели могут не отражать реальной картины улучшения вашего состояния при использовании данного медикамента. Пожалуйста, проконсультируйтесь с вашим лечащим врачом, чтобы составить график приема Ultracet Tablet. Нажмите здесь и просмотрите результаты опроса, чтобы узнать, что другие пользователи говорят о времени эффективного приема Ultracet Tablet.
-
Как часто я должен принимать Ultracet Tablet?
Пользователи TabletWise.com считают, что два раза в день и один раз в день являются наиболее оптимальной частотой приема Ultracet Tablet. Пожалуйста, проконсультируйтесь с вашим лечащим врачом, чтобы составить график приема Ultracet Tablet. Нажмите здесь и просмотрите результаты опроса, чтобы узнать, что другие пользователи говорят о частоте приема Ultracet Tablet.
-
Должен ли я использовать этот продукт на пустом желудке, перед едой или после еды?
Пользователи TabletWise.com сообщили о том, что принимают препарат Ultracet Tablet после еды. Однако, данная информация может не соответствовать вашей конкретной ситуации. Пожалуйста, проконсультируйтесь с вашим лечащим врачом, чтобы составить график приема. Нажмите здесь и просмотрите результаты опроса, чтобы узнать, что другие пользователи говорят об оптимальном времени приема Ultracet Tablet.
-
Безопасно ли управлять или эксплуатировать тяжелую технику при использовании этого продукта?
Если вы чувствуете сонливость, головокружение, гипотонию или головную боль при приеме Ultracet Tablet, то вам, возможно, стоит отказаться от управления автомобилем и тяжелым промышленным оборудованием. Вы должны отказаться от управления автомобилем, если прием препарата вызывает у вас сонливость, головокружение или гипотонию. Врачи рекомендуют отказаться от употребления алкоголя с такими препаратами, т.к. алкоголь значительно усиливает побочные эффекты и сонливость. Пожалуйста, проверьте реакцию вашего организма при приеме Ultracet Tablet. Обязательно обратитесь к вашему лечащему врачу для получения консультаций с учетом особенностей вашего организма и общего состояния здоровья.
-
Вызывает ли данный медикамент (товар) привыкание или зависимость?
Большинство препаратов не вызывают привыкания или зависимости. В большинстве случаев государство относит препараты, которые могут вызвать привыкание, к препаратам контролируемого отпуска. Например, график H или X в Индии и график II-V в США. Пожалуйста, изучите информацию на упаковке препарата, чтобы убедиться, что данный препарат не относится к категории контролируемых. Кроме того, не занимайтесь самолечением и не приучайте ваш организм к медикаментам без консультации с вашим лечащим врачом.
-
Могу ли я немедленно прекратить использование этого продукта или мне нужно медленно отменить его использование?
Прием некоторых препаратов необходимо прекращать постепенно из-за наличия эффекта восстановления. Обязательно обратитесь к вашему лечащему врачу для получения консультаций с учетом особенностей вашего организма, общего состояния здоровья и других медицинских препаратов, которые вы принимаете.
Нерегулярное применение
Если вы пропустили очередной прием лекарства, примите его как можно скорее. Если близится время очередного приема, вы можете пропустить предыдущий прием и продолжить следовать своему обычному расписанию приема медикаментов. Не принимайте дополнительную дозу препарата, чтобы компенсировать пропущенный прием. Если вы сталкиваетесь с подобной ситуацией регулярно, подумайте о возможности настройки напоминаний или попросите одного из членов вашей семьи следить за расписанием. Обязательно обратитесь к вашему лечащему врачу для корректировки расписания, чтобы компенсировать упущенный прием медикаментов (в случае, если вы пропустили значительное количество дней).
Передозировка Ultracet Tablet
- Не превышайте рекомендованную дозу. Избыточное использование препарата не облегчит ваше состояние, а также может вызвать отравление и серьезные побочные эффекты. Если вы знаете о случае передозировки Ultracet Tablet, обратитесь в службу спасения, ближайший госпиталь или больницу. Обязательно возьмите с собой упаковку, контейнер или наименование препарата, чтобы облегчить постановку диагноза.
- Не передавайте ваши препараты другим людям, даже если они находятся в том же состоянии, что и вы, или вам кажется, что ваши состояния имеют ряд схожих признаков, т.к. это может привести к передозировке.
- Пожалуйста, проконсультируйтесь с вашим лечащим врачом или фармацевтом, а также изучите информацию на упаковке изделия.
Хранение Ultracet Tablet
- Храните препараты в условиях комнатной температуры, в прохладном месте и вдали от прямых солнечных лучей. Не подвергайте препараты заморозке, если такое требование прямо отсутствует в инструкции. Храните лекарства вдали от животных и детей.
- Не смывайте препараты в туалет или дренажные системы, если такое требование прямо отсутствует в инструкции. Медикаменты, утилизируемые таким способом, могут нанести значительный вред окружающей среде. Для получения более подробной информации об утилизации Ultracet Tablet свяжитесь с вашим лечащим врачом.
Ultracet Tablet с истекшим сроком годности
- Даже один прием Ultracet Tablet с истекшим сроком годности может привести к серьезным последствиям. Обязательно обратитесь за консультацией к вашему лечащему врачу, если вы почувствуете слабость или болезненность. Кроме того, препарат с истекшим сроком годности может потерять свою эффективность в борьбе с вашим заболеванием. Для обеспечения собственной безопасности крайне важно отказаться от приема медикаментов с истекшим сроком годности. Если вы страдаете заболеванием, требующим постоянного приема медикаментов (болезни сердца, судороги, аллергические реакции, угрожающие жизни), вам необходимо наладить надежный канал связи с поставщиком вашего препарата, чтобы постоянно иметь в наличии запас свежих лекарственных средств с нормальным сроком годности.
Информация о дозировке
Пожалуйста, проконсультируйтесь с вашим лечащим врачом или фармацевтом, а также изучите информацию на упаковке изделия.
Cite эту страницу
Page URL
HTML Link
APA Style Citation
- Ultracet Tablet in русском — Товар — TabletWise.com. (n.d.). Retrieved October 15, 2023, from https://www.tabletwise.com/ru/ultracet-tablet
MLA Style Citation
- «Ultracet Tablet in русском — Товар — TabletWise.com» Tabletwise.com. N.p., n.d. Web. 15 Oct. 2023.
Chicago Style Citation
- «Ultracet Tablet in русском — Товар — TabletWise.com» Tabletwise. Accessed October 15, 2023. https://www.tabletwise.com/ru/ultracet-tablet.
Последняя дата обновления
Эта страница была обновлена на 9/27/2020.
This page provides information for Ultracet Tablet Товар in Russian.